-
CENTRES
Progammes & Centres
Location
In healthcare, one of the main rudimentary elements is health education which is lacking in India. Hygiene and cleanliness are very important as is emphasised by Prime Minister Narendra Modi and if basic habits like washing hands before eating are inculcated in the people, a lot of diseases could be prevented.
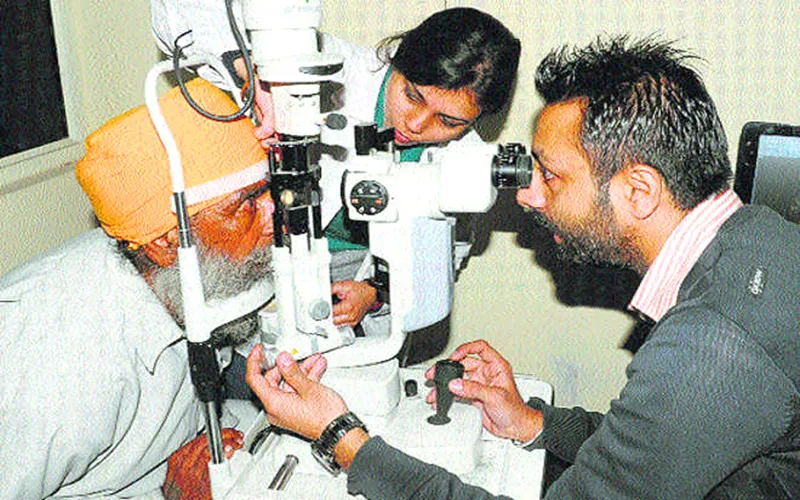
Quacks masquerading as doctors can be found everywhere in India. The recent botching up of eye surgeries in Ghuman, Batala, Punjab, is a case in point. So many people have lost their eyesight and yet public outrage would be short-lived and subdued in a few days. The victims, mostly poor, will have little recourse to justice and only paltry sums will be handed out to them as compensation. They have lost their sight, the greatest gift of all, and nothing can compensate for such a huge loss. Various committees will in the meanwhile continue with the probe.
In various hospitals and clinics all over India such botch-ups and wrong operations are an everyday affair. In the US 'malpractice' is a big offence and doctors are scared stiff of huge damages they may have to pay if malpractice suits are brought against them. In India, suing doctors is still not common and it costs money and time as well. More importantly, what the Batala incident highlights is the government's laxity in implementing any regulations or standards for the private sector's healthcare units. The government's surveillance of private hospitals in India is weak in terms of quality, reliability and cost. How could this eye camp in Ghuman go about performing eye operations without any permission from the authorities? It is not about the instruments being dirty but the whole process of running such camps reflects lack of control by the state government. It also reveals the general lack of access to public hospitals for simple eye surgeries.
The health sector in India has been in great distress for a long time. Huge big-ticket reforms are needed in hospitals by all the state governments and the Central government. First of all India spends the least amount on health as a proportion of GDP (1.1 per cent) as compared to the other members of BRICS. Public hospitals are crowded and highly congested and hence only the poor who cannot afford to go to private hospitals queue up there the whole night or at least from the early hours to get to see a specialist. Public hospitals are, however, accessible to VIPs who hog doctors' and specialists' time and hospitals' resources. They jump queues and are admitted to VIP wards immediately on arrival.
It is the lack of access to quality hospitals which forces people from low-income strata to seek free healthcare wherever it is available. In Delhi a renowned eye surgeon charges over one lakh rupees for a cataract surgery and lens implant. How many people even in the middle class can afford such high costs? In China, where the health sector was in a similar state as in India today, healthcare reforms were vigorously carried out from 2005 and it was given top priority. Today China has guaranteed healthcare for 95 per cent of the population through a health insurance cover. In India only 10 per cent people are insured for health.
Healthcare in rural areas in India is specially poor and primary health centres (PHCs), except for a few states, are under-performers and are poorly equipped with medicines, instruments, doctors and nurses. Basic healthcare has to be improved if we want a healthy India. Deprived of local healthcare, the rural population flocks to bigger hospitals in towns and cities and adds to the congestion and neglect.
In healthcare, one of the main rudimentary elements is health education which is lacking in India. Hygiene and cleanliness are very important as is emphasised by Prime Minister Narendra Modi and if basic habits like washing hands before eating are inculcated in the people, a lot of diseases could be prevented. It has been found in a survey that only 53 per cent of the people wash their hands after defecation and only 38 per cent before eating.
Since India faces multiple challenges in healthcare in the next decade, the government has to encourage the private sector. In any case the private sector has been mushrooming but the quality of treatment has to be monitored. Healthcare has become a money-making machine and the poor are scared to approach private hospitals. The doctors like in China are given to over medication and prescribe unnecessary antibiotics and imaging procedures. As a result, the patient has to bear a heavy monetary burden which makes him avoid seeking medical help. The 'out-of-pocket' expenditure in India for patients is among the highest in the world at 70 per cent. It is only 30 per cent in China.
In 2005 the government started the National Rural Health Mission and in parallel several state governments have been systematically and independently building a government-sponsored health insurance scheme to cover the costs of secondary and tertiary hospital care for the poor. The RHM has brought about an improvement in the immunisation programme and in bringing more women to hospitals for deliveries. Yet it has not been able to take care of all the health problems of the low-income population in rural areas. As a result they have to go for treatment to the private sector. Around 39 million people become poor every year due to debts incurred for medical treatment.
Huge amounts (between 39 and 42 per cent) remain unspent and unutilised under the RHM. These funds could be used in the training of medical staff as there is a big need for paramedical staff and trained nurses.
There is a scarcity of properly trained doctors and nurses in rural areas. Doctors who qualify after years of study and having invested a huge amount of money in their education, want to practice in cities and towns and many try immediately to go abroad. India is indirectly subsidising the health care system of Western countries, especially the US and the UK, by training at the public expense doctors, who then happily migrate Westwards to greener pastures.
On the whole, healthcare deserves the topmost priority of the nation and there will have to be better compliance to standards by the private healthcare industry and more widespread accreditation programme for private hospitals to prevent botch-ups.
(The writer is a Senior Fellow at Observer Research Foundation, Delhi)
Courtesy: The Tribune, December 9, 2014
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.

David Rusnok Researcher Strengthening National Climate Policy Implementation (SNAPFI) project DIW Germany
Read More +