-
CENTRES
Progammes & Centres
Location
 PDF Download
PDF Download 
Shoba Suri, “COVID-19 Compounds Global Challenges to Food Security,” ORF Issue Brief No. 485, August 2021, Observer Research Foundation.
Introduction
The COVID-19 pandemic—which has cost the world more than 4 million lives so far—has had a massive impact on global food security and nutrition. Before the end of 2019, when the first cases of the new disease were being reported from China, hundreds of millions of people across the world were already suffering from hunger and malnutrition (See Figure 1). The pandemic—and the subsequent lockdown measures that were imposed by governments as a response—have only worsened the threat to food systems, possibly hastening the impending global food emergency.[a],[1] Posing more grave threats are political conflicts, natural disasters, and other events such as locust swarms in developing regions. Food insecurity is high, and the world appears farther from meeting Sustainable Development Goal (SDG) 2 on ‘Zero hunger’.
Figure 1: The Impact of Covid-19 on SDG-2, ‘Zero Hunger’

Despite progress made over the past few decades, the triple burden of undernutrition, obesity/overweight, and diet-related micronutrient deficiencies persist in many parts of the world. Ending hunger, food insecurity, and malnutrition will require continued and focused efforts, especially in Asia and Africa—home to the largest populations that experience chronic hunger. Any progress in reducing undernutrition will have wide impacts on improving health and lifting people out of poverty.
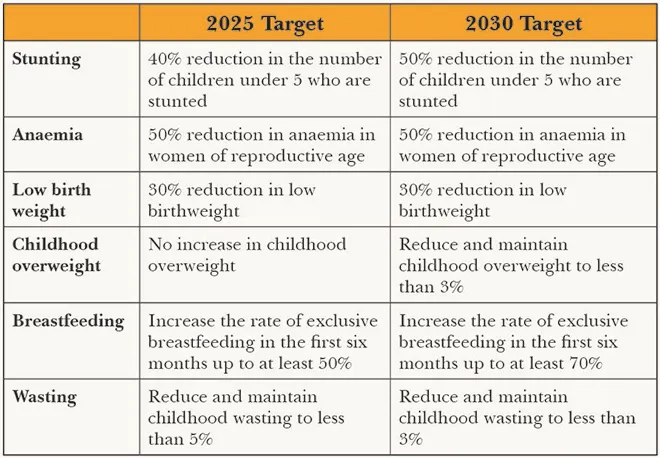
Recognising the need to accelerate action to address all forms of malnutrition, the 2012 World Health Assembly (WHA) Resolution 65.6 endorsed a comprehensive implementation plan on maternal, infant and young child nutrition. A set of six global nutrition targets (See Table 1) were specified, targeting 2.2 of the SDGs to “end all forms of malnutrition”. To align with the 2030 SDG agenda, the WHA targets were extended to 2030.[3] Looking at the rise in adult obesity and non-communicable diseases, WHA included a target to halt the rise in adult obesity and thereby reduce risk of NCD mortality by 25 percent, by 2025.[4]
Table 1: Global Nutrition Targets

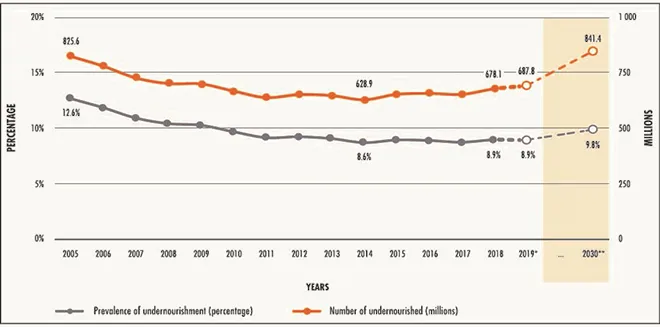
Around 690 million people or 8.9 percent of the global population are undernourished.[b],[6] (See Figure 2) Asia is home to majority of the undernourished (381 million); Africa has 250 million, and Latin America and the Caribbean follow, both with 48 million. In 2019, one in every ten people in the world (750 million) were facing severe food insecurity. Another 83 to 132 million are estimated to be added in 2020, bringing the number of undernourished to more than 840 million, or 10 percent of the population, by 2030.[7] Indeed, many countries and regions are off-track to achieve the target of ‘zero hunger’: Africa will have half of all the world’s undernourished—433 million or 51.5 percent of the population—by 2030; Asia will have 330 million (39.1 percent).[8]
Figure 2: Global undernourishment trends
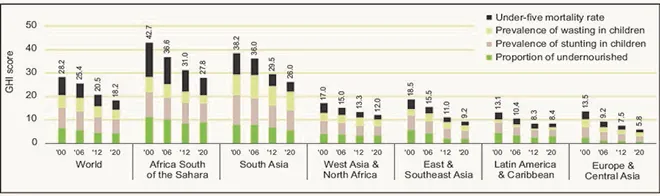
According to Global Hunger Index 2020, hunger is at moderate level worldwide.[10] Sub-Saharan Africa and South Asia have serious levels of hunger at 27.8 and 26 percent, respectively.[c] (See Figure 3)
Figure 3: Global and regional trends on Global Hunger Index 2020
Progress towards Global Nutrition Targets
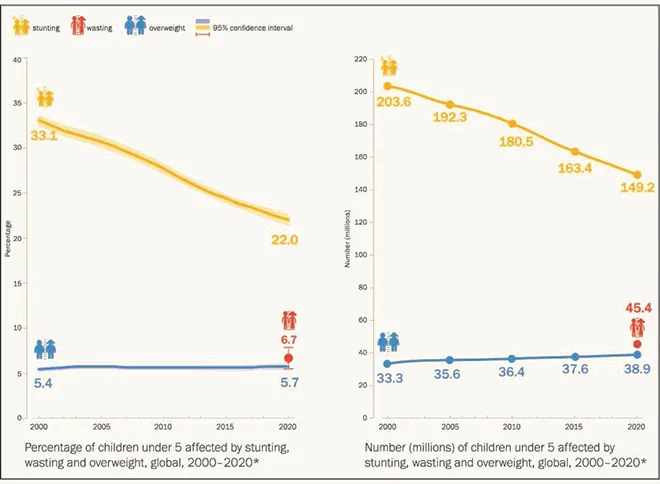
According to the Joint Malnutrition Estimate 2021, stunting has affected 149.2 million (22 percent) of all children under five years of age.[11] Wasting continues to increase at an alarming pace, reaching an estimated 45.4 million (6.7 percent) of children in 2020. A similar trend is seen in the incidence of overweight, with 38.9 million (5.7 percent) children affected in 2020. (See Figure 4)
Figure 4: Global prevalence of malnutrition, 2000-2020
To be sure, stunting rates have reduced over the past two decades. However, certain regions continue to experience high rates of stunting, and the steepest numbers are in Asia (79 million) and Africa (61.4 million). Trends indicate a significant fall in stunting rates for Sub-Saharan Africa, owing primarily to antenatal care given to mothers and increased coverage of immunisation and deworming for children under-five.[13] South Asia is the worst affected, with four out of every 10 children being stunted.[14] Among the South Asian countries, Afghanistan has the highest prevalence at 41 percent, followed by India and Pakistan both at 38 percent, and Bangladesh and Nepal both at 36 percent.[15] Stunting prevalence is almost double in children from the poorest wealth quintile, as compared to the richest quintile.
In India, there is socio-economic disparity in the burden of malnutrition in households.[16],[17] Between 2006 and 2016, adult overweight/obesity doubled as wealth inequalities increased in both rural and urban slum households.[18] Overall, in South Asia, there are multiple factors that account for variance in child stunting rates: dietary diversity, maternal education, and degree of household poverty. [19] Moreover, poor infant and young child feeding and poor maternal nutrition and sanitation contribute to stunting in South Asia and Sub-Saharan Africa. [20]
Globally, 45.4 million (6.7 percent) children under-five are wasted, far higher than the SDG-30 and Global Nutrition targets of 3 percent and 5 percent, respectively. (See Table 1)[21] South Asia accounts for 70 percent (31.9 million) of under-five wasting and more than a quarter (27 percent) live in Africa. Of the 31.9 million children affected by wasting in Asia, more than half live in South Asia (25 million). A study in South Asia found that the actors associated with wasting among children under-five include low maternal body mass index, short maternal height, high number of poorest wealth quintile households, and lack of maternal education.[22],[23]
The prevalence of child wasting at 14.8 percent in South Asia is a cause of concern and calls for prioritising action in improving nutrition and healthcare for women before and during pregnancy not only to prevent low birth weight, but importantly, for their own health and well-being.[24] Child wasting across low-and middle-income countries peak at 0-3 months and is prevalent at 12-15 months.[25] This necessitates preventive interventions in pregnant and lactating mothers, and for children below six months of age. New estimates suggest a 14.3-percent (6.7 million) rise in child wasting in 2020, about 58 percent children in South Asia and about 22 percent in sub-Saharan Africa. [26] As countries continue to grapple with the effects of COVID-19 on livelihoods, an additional 3.9 million children in South Asia could suffer from wasting.[27]
The burden of overweight in both under-fives and in adults has been on the rise.[28] Globally, about 38.9 million (5.7 percent) of children under-five are overweight. Almost half of the total live in Asia (18.7 million); the other big proportion is in Africa (10.6 million). Trends indicate a significant increase in overweight children in Southeast Asia and Northern Africa in the past two decades. The number increased from 2 million to 4.2 million in Southeastern Asia, and from 2.3 million to 3.8 million children in Northern Africa between 2000 to 2020. Increasing trends have been observed for the sub-regions of Australia and New Zealand (16.9 percent), and Northern America (9.1 percent). Most regions are not on-track to achieve the targets on overweight in children. Indeed, the global prevalence in under-fives has seen no progress in two decades.
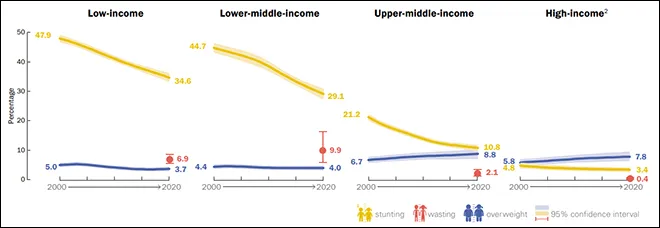
Figure 5 indicates the percentage of children affected by all forms of malnutrition by income classification of countries. While stunting is on the decline for all income levels, overweight is rising at an alarming pace especially in upper-middle and high-income countries. Almost two-thirds (72 percent) of wasted children under-five are in low- and middle-income countries, as compared to 59 percent of stunted children.
Figure 5: Under-fives affected by stunting, wasting and overweight, by country income classification, 2000–2020
Of all other global targets, exclusive breastfeeding is the only indicator that appears to be on-track to achieve at least the 50-percent rate by 2025 (See Figure 6). At present, 44 percent of children are exclusively breastfed worldwide, with South Asia and East and Southern Africa above the global average at 57 percent and 56 percent, respectively. If the regions continue at the same pace, they might be able to achieve both SDG and global targets. Most subregions have made some progress, except for Latin America and the Caribbean.
Figure 6: Progress on Global Nutrition Targets
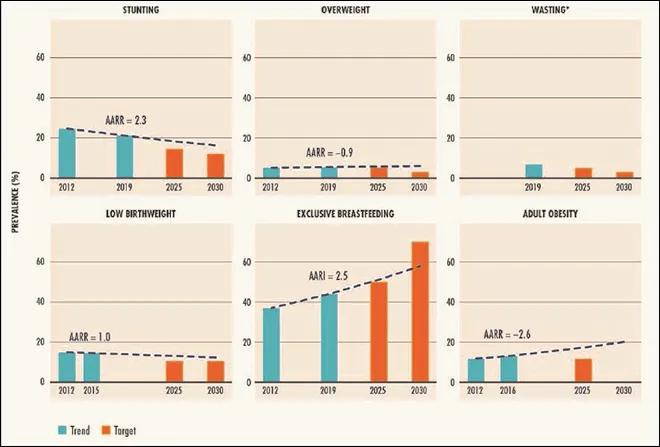
Nearly 15 percent of infants born worldwide are of low birth weight (less than 2500 gm). Progress on the reduction of low birth weight has been stagnant for the past decades.[31] South Asia, Sub-Saharan Africa, and Latin America are the top three regions with the highest prevalence of low birth weight at 28, 13, and 9 percent, respectively. There has been slow progress in achieving the target of 30-percent reduction in low birth weight by 2030. Multiple pregnancies, infections, and non-communicable diseases can cause low birth weight with adverse consequences, such as neonatal mortality, poor cognitive development and future risk of cardiovascular diseases.[32],[33] Interventions to improve early and continued access to high-quality antenatal care and perinatal services, nutritional counselling, along with early essential newborn care are critical for preventing and treating low birth weight. [34],[35]
Adult obesity continues to rise across all subregions, and has tripled in the past four decades.[36] Worldwide, about 13 percent of the adult population (11 percent of males and 15 percent of females) are obese.[37] Overweight and obesity is the fifth leading cause of global deaths.[38] It also contributes to the rise in risk factor for non-communicable diseases such as cardiovascular disease, diabetes, and certain cancers.[39]
COVID-19 is undermining nutrition and health efforts across low- and middle-income countries and worst affected are women and children, with the interruption of nutrition services and poor quality of diet pushing women and children into malnutrition.[40] The pandemic has brought an additional 140 million people to extreme poverty, living on less than US$1.90 per day in 2020. [41]
The World Food Programme estimated that the food-insecure population would go up to 265 million by end of 2020 along with a decline in access to child health and nutrition services.[42] A 30-percent reduction is estimated in the coverage of nutrition services due to lockdowns and the disruption of supply chains. [43] Lancet estimates a minimum need of US$2.4 billion for four life-saving interventions: prevention of wasting in children at risk; treatment for children who are wasted; biannual vitamin A supplementation for children aged 6–59 months (90-percent coverage); and mass communication for the protection, promotion, and support of breastfeeding that focuses on caregivers or families of children aged 0–23 months. [44]
SDG 2 ‘Zero Hunger’: Why it Matters
To eradicate hunger, the SDG 2 targets need to be aligned to the four main dimensions of food security: food availability, access to food, food utilisation, and the overall stability of the three dimensions.
The rapidly shifting food value chain and diet of low- and middle-income countries, urbanisation, and move towards increased consumption of packaged foods have challenged food systems and the health of the poor.[45] Extreme hunger and malnutrition remains a barrier to sustainable development and the pandemic has further added to constraints in income and other resources. Climate shocks and locust crises also worsen food insecurity.[46],[47]
It is crucial to invest in agriculture and sustainable food production to lessen the hunger threat, improve food security, and build resilience to disasters and shocks.[48] Achieving ‘zero hunger’ will have positive impacts not only on health, but also on the economy, education, equality, and social development. Sustained investment to improve access to food in both rural and urban areas, along with social protection, can help in the recovery.[49]
The World Food Summit of 1996 declared: “Food security exists when all people, at all times, have physical and economic access to sufficient safe and nutritious food that meets their dietary needs and food preferences for an active and healthy life.”[50] Even before the pandemic, about 2 billion people were already at risk of moderate to severe food insecurity. COVID-19 has further undermined efforts to achieve the SDG on ‘zero hunger’.
The World Health Organization (WHO) warns that the situation can worsen as experts predict that it will take more time before the pandemic abates.[51],[52] Food productivity could also be affected in the future, especially if the virus is not contained and the lockdown measures continue.[53] Both malnutrition and overnutrition cause the immune system to weaken, making the person vulnerable to COVID-19 and setting off a vicious cycle of illness and hunger.[54] Disruption to the already inequitable health and nutrition services have had a severe impact on the poor and vulnerable.[55] Increased vulnerability from micronutrient deficiencies and pre-existing medical conditions have been aggravated during the pandemic.[56]
Figure 7: How COVID-19 affects food security and nutrition
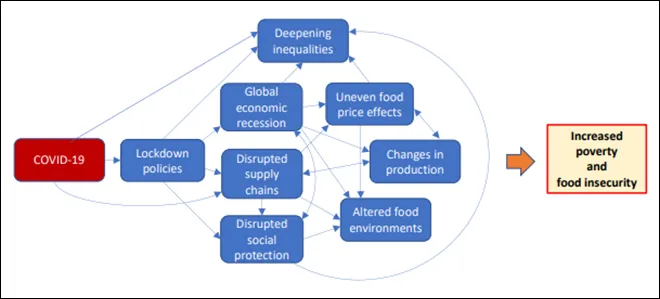
Lockdown and other containment measures have worsened loss of incomes, disruption in food supply chain and social protection, deepening inequality, and leading to uneven food prices (See Figure 7).[58],[59] The supply chain disruption has led to wastage, as demand dropped and farmers with inadequate storage were left with food they could not sell.[60] Countries with high prevalence of food insecurity were highly affected by the disruptions in supply chains.[61] Food production cycles that relied on migrant labour were affected due to travel restrictions and the closing down of work facilities to contain the outbreak.[62]
Global economic recession and the associated income reduction have led to loss of livelihood, causing a drop in purchasing power that in turn has resulted in food insecurity.[63] About 400 million full-time jobs were lost in 2020 due to lockdown measures.[64] Similarly, around one-third of food system livelihoods are at risk due to the pandemic. [65]
The economic slowdown has worsened existing inequalities, and has had an impact on food security.[66],[67] With one in every three people lacking access to safe drinking water and handwashing facilities, there is a high likelihood of contracting infections.[68],[69] Unsafe work conditions, low wages, and lack of protective equipment have further added to the woes of workers.[70] Women have faced additional burdens as frontline workers, unpaid care workers, and food system workers.[71],[72] Furthermore, there has been increased incidence of domestic violence due to the pressures of lost livelihoods and forced confinement at home.[73],[74]
Cash or food transfers are crucial for the vulnerable to cope with the economic and health exposures caused by the crisis. Around 90 percent of women in Asia and Africa work in the informal sector and lack social protection.[75] There are other challenges to cash transfer programmes in India, Pakistan, and Tanzania, with women often unaware of their benefits and entitlements.[76],[77],[78] The closure of schools during the lockdown have led to disruption of the school meal porgramme, affecting the nutrition of some 370 million children.[79]
The pandemic has altered the overall food environment as countries shut down informal food markets, which were seen as source of disease transmission.[d] Households have made a shift with consumption of calorie-rich staple foods instead of high-micronutrient fruits and vegetables.[80] There has also been a shift towards consumption of more processed foods.[81] The renewed interest in community-supported agriculture and home gardening to grow their own fruits and vegetables, can help to ensure food security and diversity. [82],[83]
Food price increases have also resulted from disrupted supply chains that have affected the cost of shipping.[84] High retail prices and reduced incomes have forced more households to cut down on the quantity and quality of their food.[85] These localised price increases directly impact food security and nutrition as food becomes more difficult to access, especially for the poor.
A 2020 rapid phone survey by the World Bank in 48 countries found reduced food consumption and compromised nutrition by families.[86] The crisis has affected the food production with disruption in supply chain of agricultural inputs such as seeds and fertiliser, making them scarce and thus more expensive.[87],[88] Coordinated action within the food system – production, trade and distribution, and consumption—can significantly reduce economic and food insecurity in populations affected by the pandemic, and support rapid recovery.[89]
Recommendations and Conclusion
Policymakers must step up efforts to eliminate all forms of malnutrition and break the intergenerational cycle of poverty. It is estimated that scaling up high-impact, nutrition-specific interventions in all low- and middle-income countries could generate about $417 billion in economic benefits and result in a 40-percent decline in stunting.[90] Every $1 invested in stunting reduction will generate $11 in economic returns. More sectors and actors, beyond health and agriculture, need to be involved.
A “food systems” approach to malnutrition requires inclusive policies that will address both supply and demand. It is necessary to reinforce strategic action to address people’s needs, now and as the crisis abates, to build a resilient food system. While daunting and exacting a heavy toll, pandemics can serve as a turning point to rebalance and transform food systems, making them more inclusive, sustainable, and resilient.[91] Governments should address short-term problems and also those necessary for building longer-term resilience.
First, nations must implement policies and channel investments for reducing the cost of nutritious food. The imperative is for policies and programmes that will mainstream nutrition across all sectors, beyond health and agriculture. Working towards the global nutrition targets requires inclusive, sustainable and efficient food systems that deliver nutritious food. Urgent action is required to ensure access to the poorest of the poor. Policies need to be aligned towards a nutrition-sensitive value chain to enhance efficiencies in food storage, processing, packaging, distribution and marketing, thereby reducing food losses.
Second, to mitigate the societal disruption and economic shocks caused by the pandemic, more robust social protection programmes need to be initiated to improve access to healthy and nutritious food. Investing in social protection can be instrumental in strengthening people’s access to food and essential services, particularly for vulnerable groups in both urban and rural settings. There should be better protections for vulnerable and marginalised food system workers and farmers who are disproportionately affected by the crisis. All together, the social protection, healthcare, and food systems can work to meet people’s nutritional needs. Such protections would strengthen the resilience of food systems in the face of crises such as that unleashed by COVID-19.
Third, sustainable and inclusive economic growth must be promoted to create more job opportunities and improve living standards. The pandemic has disrupted lives and livelihoods and jeopardised the global economy. Empowering women will be key to improved nutrition, as they play a decisive role in their family’s food security.
The global 2030 nutrition agenda calls for transformational change and collaborative work to develop strategies, cost-effective interventions and investments in nutrition. These are needed, along with poverty reduction, the empowerment of women, and improvements in maternal health.
[a] A food emergency is defined as “an extraordinary situation in which people are unable to meet their basic survival needs, or there are serious and immediate threats to human life and well-being.”
[b] ‘Undernourished’ means not having enough food or enough of the right type of food.
[c] GHI scores the share of people who are undernourished, child wasting rate, child stunting rate, and child mortality rate.
[d] The ground-zero of SARS-CoV-2 was a wet market in Wuhan.
[1] UN 2020, Policy Brief: The impact of Covid-19 on Food security and Nutrition, https://reliefweb.int/sites/reliefweb.int/files/resources/sg_policy_brief_on_covid_impact_on_food_security.pdf
[2] The Sustainable Development Goals Report 2020, https://unstats.un.org/sdgs/report/2020/The-Sustainable-Development-Goals-Report-2020.pdf
[3] Transforming our world: the 2030 Agenda for Sustainable Development, https://sdgs.un.org/2030agenda
[4] World Health Organization 2016, Global NCD target halt the rise in Obesity, https://www.who.int/beat-ncds/take-action/policy-brief-halt-obesity.pdf
[5] The state of food security and nutrition in the world 2020: transforming food systems for affordable healthy diets. Vol. 2020. Food & Agriculture Org., 2020,http://www.fao.org/3/ca9692en/ca9692en.pdf
[6] In Brief: The state of food security and nutrition in the world 2020: transforming food systems for affordable healthy diets. Vol. 2020. Food & Agriculture Org., 2020,https://www.unicef.org/media/72686/file/SOFI-2020-in-brief.pdf
[7] The state of food security and nutrition in the world 2020
[8] World Health Organization News 2020, https://www.who.int/news/item/13-07-2020-as-more-go-hungry-and-malnutrition-persists-achieving-zero-hunger-by-2030-in-doubt-un-report-warns
[9] The state of food security and nutrition in the world 2020
[10] Global Hunger Index 2021, https://www.globalhungerindex.org/trends.html
[11] UNICEF/WHO/The World Bank Group Joint Child Malnutrition Estimates: levels and trends in child malnutrition: key findings of the 2021 edition. (2021),https://www.who.int/publications/i/item/9789240025257
[12] UNICEF / WHO / World Bank Group Joint Child Malnutrition Estimates 2021
[13] Buisman, Leander R., Ellen Van de Poel, Owen O’Donnell, and Eddy KA van Doorslaer. “What explains the fall in child stunting in Sub-Saharan Africa?.” SSM-population health 8 (2019): 100384,https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6545382/
[14] UNICEF-Stop Stunting. South Asis Headline Results 2018-21, http://www.unicefrosa-progressreport.org/stopstunting.html
[15] Miki Terasawa, ‘Tackling malnutrition in South Asia: 8 years on’. World Bank Blogs, April 30, 2019, https://blogs.worldbank.org/endpovertyinsouthasia/tackling-malnutrition-south-asia-8-years#:~:text=Afghanistan%20has%20the%20highest%20rate,and%20Nepal%20at%2036%20percent.
[16] Nakphong, Michelle K., and Hiram Beltrán-Sánchez. “Socio-economic status and the double burden of malnutrition in Cambodia between 2000 and 2014: overweight mothers and stunted children.” Public health nutrition 24, no. 7 (2021): 1806-1817,https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8094435/
[17] Nguyen, Phuong Hong et al., “The double burden of malnutrition in India: Trends and inequalities (2006–2016),” Plos One 16, no. 2 (2021): e0247856,https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0247856
[18] Nguyen, Phuong Hong et al., “The double burden of malnutrition in India.”
[19] Krishna, Aditi et al.,”Trends in inequalities in child stunting in South Asia.” Maternal & Child Nutrition 14 (2018): e12517, https://www.researchgate.net/publication/320499467_Trends_in_inequalities_in_child_stunting_in_South_Asia
[20] Smith, Lisa C., and Lawrence Haddad. “Reducing child undernutrition: past drivers and priorities for the post-MDG era.” World Development 68 (2015): 180-204,https://www.sciencedirect.com/science/article/pii/S0305750X14003726
[21] UNICEF / WHO / World Bank Group Joint Child Malnutrition Estimates 2021.
[22] Harding, Kassandra L., Victor M. Aguayo, and Patrick Webb. “Factors associated with wasting among children under five years old in South Asia: Implications for action.” PloS one 13, no. 7 (2018): e0198749,https://pubmed.ncbi.nlm.nih.gov/29969457/
[23] Li, Zhihui et al.,”Factors associated with child stunting, wasting, and underweight in 35 low-and middle-income countries.” JAMA network open 3, no. 4 (2020): e203386-e203386,https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2764662
[24] Torlesse, Harriet, and Minh Tram Le. “South Asia and child wasting–unravelling the conundrum.” Field Exchange 63 (2020): 7,https://www.ennonline.net/fex/63/southasiachildwasting
[25] Mertens, Andrew et al., “Child wasting and concurrent stunting in low-and middle-income countries.” medRxiv (2020),https://www.medrxiv.org/content/10.1101/2020.06.09.20126979v1
[26] Headey, Derek et al., “Impacts of COVID-19 on childhood malnutrition and nutrition-related mortality.” The Lancet 396, no. 10250 (2020): 519-52,1.https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)31647-0/fulltext#back-bib11
[27] Headey, Derek et al., “Impacts of COVID-19 on childhood malnutrition and nutrition-related mortality.”
[28] UNICEF / WHO / World Bank Group Joint Child Malnutrition Estimates 2021.
[29] UNICEF / WHO / World Bank Group Joint Child Malnutrition Estimates 2021.
[30] The state of food security and nutrition in the world 2020.
[31] World Health Organization. Global Nutrition Targets 2025: Low birth weight policy brief. No. WHO/NMH/NHD/14.5. World Health Organization, 2014,http://apps.who.int/iris/bitstream/handle/10665/149020/WHO_NMH_NHD_14.5_eng.pdf?ua=1
[32] Larroque, Béatrice et al.,”School difficulties in 20-year-olds who were born small for gestational age at term in a regional cohort study.” Pediatrics 108, no. 1 (2001): 111-115,https://pubmed.ncbi.nlm.nih.gov/11433062/
[33] Risnes, Kari R et al. “Birthweight and mortality in adulthood: a systematic review and meta-analysis.” International journal of epidemiology 40, no. 3 (2011): 647-661,https://pubmed.ncbi.nlm.nih.gov/21324938/
[34] Technical Brief 2018. Saving lives and giving newborns the best start: Critical nutrition interventions for mothers and infants in the perinatal period, https://www.healthynewbornnetwork.org/hnn-content/uploads/Saving-lives-and-giving-newborns-the-best-start.pdf
[35] Global Nutrition Target 2025, https://apps.who.int/iris/rest/bitstreams/665585/retrieve
[36] World Health Organization 2021. Obesity & Over weight-Key Facts, https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight#:~:text=Of%20these%20over%20650%20million%20adults%20were%20obese.,tripled%20between%201975%20and%202016.
[37] World Health Organization Noncommunicable diseases – High-level action needed to meet the SDGs and beat NCDs, https://www.who.int/beat-ncds/take-action/targets/en/#:~:text=Target%201%3A%20A%2025%25%20relative,diabetes%2C%20or%20chronic%20respiratory%20diseases.&text=Target%202%3A%20At%20least%2010,appropriate%2C%20within%20the%20national%20context.
[38] The European association for Study of Obesity. Obesity Statistics, https://easo.org/media-portal/statistics/#:~:text=65%25%20of%20the%20world’s%20population,of%20being%20overweight%20or%20obese.
[39] World Health Organization 2021. Obesity & Over weight-Key Facts.
[40] Fore, Henrietta H et al., “Child malnutrition and COVID-19: the time to act is now.” The Lancet 396, no. 10250 (2020): 517-518,https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)31648-2/fulltext
[41] Laborde, David, Will Martin, and Rob Vos. “Poverty and food insecurity could grow dramatically as COVID-19 spreads.” International Food Policy Research Institute (IFPRI), Washington, DC (2020),https://www.ifpri.org/blog/poverty-and-food-insecurity-could-grow-dramatically-covid-19-spreads
[42] World Food Programme. “COVID-19 will double number of people facing food crises unless swift action is taken.” Media release (2020),https://www.wfp.org/news/covid-19-will-double-number-people-facing-food-crises-unless-swift-action-taken
[43] Tracking the situation of children during Covid-19. UNICEF Dashboard 2021, https://data.unicef.org/resources/rapid-situation-tracking-covid-19-socioeconomic-impacts-data-viz/
[44] Fore, Henrietta H., Qu Dongyu, David M. Beasley, and Tedros A. Ghebreyesus. “Child malnutrition and COVID-19: the time to act is now.” The Lancet 396, no. 10250 (2020): 517-518.
[45] Popkin, Barry M. “Nutrition, agriculture and the global food system in low and middle income countries.” Food policy 47 (2014): 91-96.https://www.sciencedirect.com/science/article/abs/pii/S030691921400075X
[46] FAO. 2021. The impact of disasters and crises on agriculture and food security: 2021 Rome, https://doi.org/10.4060/cb3673enhttp://www.fao.org/3/cb3673en/cb3673en.pdf
[47] Fact Sheet, ‘The Locust Crisis: the World Bank’s Response’, 1 July 2020, https://www.worldbank.org/en/news/factsheet/2020/04/27/the-locust-crisis-the-world-banks-response
[48] FAO 2021. The impact of disasters and crises on agriculture and food security.
[49] Zero Hunger-Why it matters, http://cdn.worldslargestlesson.globalgoals.org/2017/03/2.pdf
[50] World Food Summit 1996. Rome Declaration on World Food Security, http://www.fao.org/3/w3613e/w3613e00.htm
[51] WHO on Coronavirus:’the worst is yet to come’. 30 June 2020, https://www.youtube.com/watch?v=l-lx6ZYQ_vg
[52] Scudellari, Megan. “How the pandemic might play out in 2021 and beyond.” Nature (2020): 22-25,https://www.nature.com/articles/d41586-020-02278-5
[53] HLPE 2020. Impacts of COVID-19 on food security and nutrition: developing effective policy responses to address the hunger and malnutrition pandemic, https://doi.org/10.4060/cb1000en
[54] Global Nutrition Report 2020, https://globalnutritionreport.org/blog/nutrition-and-covid-19-malnutrition-threat-multiplier/
[55] Muhammad AP & Martien VN, ‘How nutrition can portect people’s health during Covid-19’, World Bank Blogs, 13 May 2020. https://blogs.worldbank.org/voices/how-nutrition-can-protect-peoples-health-during-covid-19
[56] McAuliffe, Shane et al.,”Dietary micronutrients in the wake of COVID-19: an appraisal of evidence with a focus on high-risk groups and preventative healthcare.” BMJ nutrition, prevention & health 3, no. 1 (2020): 93,https://nutrition.bmj.com/content/early/2020/06/17/bmjnph-2020-000100
[57] UN 2020. Policy Brief: The impact of Covid-19 on Food security and Nutrition.
[58] Klassen, Susanna, and Sophia Murphy. “Equity as both a means and an end: lessons for resilient food systems from COVID-19.” World Development 136 (2020): 105104,https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7402645/
[59] Laborde, David, W. Martin, and R. Vos. “Estimating the poverty impact of COVID-19: The MIRAGRODEP and POVANA frameworks.” IFPRI Technical Note, IFPRI.(also available at https://tinyurl. com/y9fazbzf) (2020),https://www.researchgate.net/publication/342068871_Estimating_the_Poverty_Impact_of_COVID-19_The_MIRAGRODEP_and_POVANA_frameworks_1
[60] Clapp, Jennifer, and William G. Moseley. “This food crisis is different: COVID-19 and the fragility of the neoliberal food security order.” The Journal of Peasant Studies 47, no. 7 (2020): 1393-1417,https://www.tandfonline.com/doi/full/10.1080/03066150.2020.1823838
[61] FAO, IFAD, UNICEF, WFP and WHO. 2019. The State of Food Security and Nutrition in the World 2019. Safeguarding against economic slowdowns and downturns. Rome, FAO,https://www.wfp.org/publications/2019-state-food-security-and-nutrition-world-sofi-safeguarding-against-economic
[62] Haley, Ella et al., “Migrant farmworkers face heightened vulnerabilities during COVID-19.” Journal of Agriculture, Food Systems, and Community Development 9, no. 3 (2020): 35-39,https://www.foodsystemsjournal.org/index.php/fsj/article/view/810
[63] Global Economic Prospects. A World Bank Group Flagship Report 2021, https://www.worldbank.org/en/publication/global-economic-prospects#overview
[64] ILO Monitor: COVID-19 and the world of work. Fifth edition Updated estimates and analysis 2020, https://www.ilo.org/wcmsp5/groups/public/@dgreports/@dcomm/documents/briefingnote/wcms_749399.pdf
[65] UN 2020. Policy Brief: The impact of Covid-19 on Food security and Nutrition.
[66] Ashford, NA et al., “Addressing inequality: the first step beyond COVID-19 and towards sustainability.” Sustainability 12, no. 13 (2020): 5404,https://www.mdpi.com/2071-1050/12/13/5404
[67] Klassen, Susanna, and Sophia Murphy. “Equity as both a means and an end.”
[68] World Health Organization News 2019, https://www.who.int/news-room/detail/18-06-2019-1-in-3-people-globally-do-not-have-access-to-safe-drinking-water-unicef-who
[69] Ekumah, B et al.,”Disparate on-site access to water, sanitation, and food storage heighten the risk of COVID-19 spread in Sub-Saharan Africa.” Environmental research 189 (2020): 109936,https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7368919/
[70] Klassen, Susanna, and Sophia Murphy. “Equity as both a means and an end”.
[71] Power, Kate. “The COVID-19 pandemic has increased the care burden of women and families.” Sustainability: Science, Practice and Policy 16, no. 1 (2020): 67-73.
[72] McLaren et al., “Covid-19 and women’s triple burden: Vignettes from Sri Lanka, Malaysia, Vietnam and Australia.” Social Sciences 9, no. 5 (2020): 87.
[73] World Health Organization. Gender and COVID-19: advocacy brief, 14 May 2020. No. WHO/2019-nCoV/Advocacy_brief/Gender/2020.1. World Health Organization, 2020.
[74] FAO 2020. Gendered impacts of COVID-19 and equitable policy responses in agriculture, food security and nutrition, http://www.fao.org/documents/card/en/c/ca9198en.
[75] Women and men in the informal economy: a statistical picture (third edition) / International Labour Office – Geneva: ILO, 2018,https://www.ilo.org/global/publications/books/WCMS_626831/lang–en/index.htm
[76] Simone Schaner. Enhancing Women’s Economic Empowerment Through Digital Cash Transfers: Analysis of the Digitize/Direct/Design Criteria Applied to the National Rural Employment Guarantee Scheme in Bihar, India. Harvard Kennedy School 2019, https://www.findevgateway.org/sites/default/files/publications/files/_d3_final_report_bihar.pdf
[77] Enhancing Women’s Economic Empowerment Through Digital Cash Transfers: What Do We Learn from the Digitize/Direct/Design (D3) Criteria in the Case of Benazir Income Support Program in Pakistan? IDEATE 2018,
https://www.findevgateway.org/sites/default/files/publications/files/_d3_final_report_pakistan_bisp.pdf
[78]Flora Myamba and Caroline Pulver, 2019. Enhancing Women’s Economic Empowerment Through Digital Cash Transfers: Digitize/Direct/Design (D3) Criteria – An Application to Tanzania, https://www.findevgateway.org/sites/default/files/publications/files/_d3_final_report_tanzania.pdf
[79] World Food Programme 2020. Global Monitoring of School Meals during COVID-19 Closures, https://cdn.wfp.org/2020/school-feeding-map/
[80] Glauber, Joseph, David Laborde Debucquet, Will Martin, and Rob Vos. “COVID-19: Trade restrictions are worst possible response to safeguard food security.” IFPRI book chapters (2020): 66-68.
[81] Bracale, Renata, and Concetta M. Vaccaro. “Changes in food choice following restrictive measures due to Covid-19.” Nutrition, Metabolism and Cardiovascular Diseases 30, no. 9 (2020): 1423-1426.
[82] Worstell, James. “Ecological resilience of food systems in response to the COVID-19 crisis.” Journal of Agriculture, Food Systems, and Community Development 9, no. 3 (2020): 23-30,https://www.foodsystemsjournal.org/index.php/fsj/article/view/806
[83] Lal, Rattan. “Home gardening and urban agriculture for advancing food and nutritional security in response to the COVID-19 pandemic.” Food security (2020): 1-6,https://link.springer.com/article/10.1007/s12571-020-01058-3
[84] FAO. 2020 Food Outlook – Biannual Report on Global Food Markets: June 2020. Food Outlook, 1. Rome, https://doi.org/10.4060/ca9509en.
[85] The World Bank Brief 2021. Food Security and Covid 19, https://www.worldbank.org/en/topic/agriculture/brief/food-security-and-covid-19
[86] World Bank 2020. Covid-19 Household Monitoring Dashboard, https://www.worldbank.org/en/data/interactive/2020/11/11/covid-19-high-frequency-monitoring-dashboard
[87] Pu, Mingzhe, and Yu Zhong. “Rising concerns over agricultural production as COVID-19 spreads: Lessons from China.” Global food security 26 (2020): 100409.
[88] Arouna, Aminou, Guillaume Soullier, Patricio Mendez Del Villar, and Matty Demont. “Policy options for mitigating impacts of COVID-19 on domestic rice value chains and food security in West Africa.” Global Food Security 26 (2020): 100405.
[89] HLPE 2020.
[90] TARGET, STUNTING. “An Investment Framework for Meeting the Global Nutrition Target for Stunting,” https://openknowledge.worldbank.org/bitstream/handle/10986/26069/Stunting_5_web.pdf?sequence=8&isAllowed=y
[91] UN 2020. Policy Brief: The impact of Covid-19 on Food security and Nutrition.
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.

Dr. Shoba Suri is a Senior Fellow with ORFs Health Initiative. Shoba is a nutritionist with experience in community and clinical research. She has worked on nutrition, ...
Read More +