-
CENTRES
Progammes & Centres
Location

South Asian countries have been typically known for the high population density, with a large number of people surviving in compact spaces in urban slums and rural areas, making it a typical breeding ground for the Novel Coronavirus pandemic. Home to a half of the world’s multidimensionally poor people in 2017, South Asian countries lack in various health and nutrition indicators, with inadequate public healthcare facilities. Some of South Asia’s human development indicators, especially in the area of nutrition, have been worse than Sub-Saharan Africa, despite impressive poverty reduction and better economic growth, resulting in experts calling it the “South Asian Enigma”. The persisting inequality and gaps in provision of basic amenities further cemented the belief that Covid-19 could be deadly for this region. However, six months into the Covid-19 pandemic, South Asia’s fatality rates have left most confused.
One month into the pandemic, the world’s most developed economies witnessed an unprecedented surge in Covid-19 cases as well as deaths, seemingly unable to cope with the virus. Meanwhile, the South Asian region—comprising of Afghanistan, Bangladesh, Bhutan, India, Maldives, Nepal, Pakistan and Sri Lanka—when compared to the North American, East Asian or Western European region saw far lesser infections and deaths. On April 20th, South Asia, while accounting for 23.4 percent of the world’s population, only contributed to 1.25 percent of the infections, and 0.5 percent to the deaths. Interestingly, Africa’s morbidity and mortality burden from COVID-19 are similarly low, with experts talking about an “African Enigma” as well.
As of September 15th 2020, South Asia contributes to 19 percent of the global reported cases and 10 percent to the global reported deaths, skewed due to India’s contribution of 87 percent of South Asia’s cases and 86 percent to South Asia’s deaths. When taking into consideration the large population size of South Asia, it seems to show a somewhat optimistic figure of 3,054 infections per million population and 50 deaths per million population, on completion of half a year of the pandemic.
It has been argued that the low numbers could have been the result of a delayed onset of community transmission in these countries, and perhaps an earlier adoption of country-wide lockdowns and international travel bans, given the healthcare system deficit. It has also been hypothesized that the mandatory BCG vaccination against Tuberculosis or the prevalence of other coronaviruses in these countries could have strengthened the immune system. On the other hand, lack of testing kits and infrastructure, leading to testing of symptomatic patients only, could also partly explain this paradoxical situation. However, it remains clear that death rates in South Asia remain surprisingly low.
A look at the South Asian countries reveals that, while cases have been rising and seem frightening when observed in absolute terms, the same numbers when looked at as population proportions reveal a different story. Graph 1 shows a comparison of the cases and deaths per million population in South Asian countries and the Top 10 most infected countries (except India). South Asian countries clearly indicate a lower spread of infection and the subsequent deaths caused by the disease. The most infected country with respect to population, Peru’s deaths per million population (932) is 15 times higher than that of the most infected South Asian Country, Maldives (61). The low number of infections in South Asia could be hypothesized to be a result of low testing, but the lower number of deaths indicate a different story altogether.
Figure 1: South Asia Novel Coronavirus case per million population v/s deaths per million population
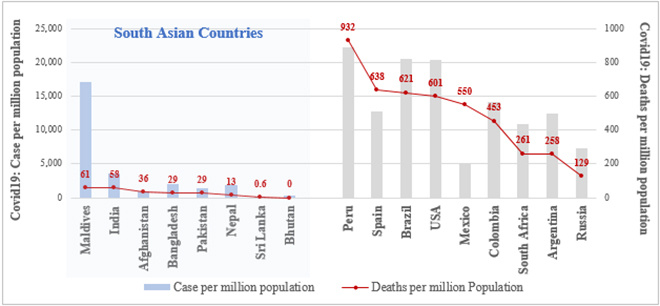 Data as of September 15, 2020, Source: https://www.worldometers.info/coronavirus/
Data as of September 15, 2020, Source: https://www.worldometers.info/coronavirus/
Currently, only three out of the eight South Asian countries—namely, India, Bangladesh and Pakistan—are in the top 20 most infected countries across the world. In terms of deaths, India is the only one to be in the top 20 list of the world.
A Sub-Country Analysis
When comparing the case and death per million population, Maldives seems to be performing badly, but these numbers can be misleading due its very low population base making clusters of cases result in higher per population figures. In absolute terms, Maldives seems to be performing adequately, considering the limited health infrastructure. The Covid-19 trend line (graph 2) seems to be showing a gradual flattening of the curve. While the nation seems to be strongly fighting and coping with the virus, the pandemic has offset other alarming issues. Two-thirds of the country’s GDP is generated through its tourism industry, and the worldwide lockdown, travel bans and panic may threaten the country’s immediate economic future.
Figure 2: Covid-19 confirmed cases: Trajectory of South Asian Countries
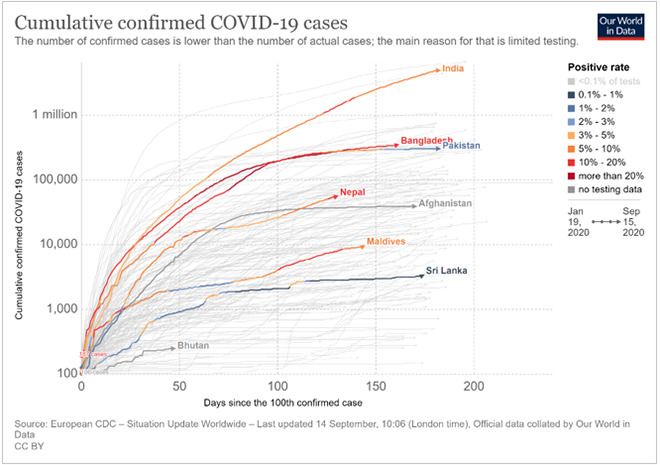 Data as of September 15, 2020, Source: https://ourworldindata.org/covid-cases
Data as of September 15, 2020, Source: https://ourworldindata.org/covid-cases
India, while showing surprisingly low levels of infections and deaths during the initial few months of the pandemic, has now become the second most infected country in terms of cases, and third in terms of deaths. India has a population of 1.3 billion, therefore the high number of cases in country vis-à-vis rest of its South Asian counterparts is not surprising. The figures when adjusted for population seem less alarming, but the rising number of cases and deaths in India is concerning nevertheless. Graph 2 shows the upward trend in India’s infections, without any particular sign of a flattening in the near future. The entire month of September has observed record-high increase in daily cases (more than ~90,000) and deaths (more than ~1000). Although cases and deaths are steadily rising in India, it is imperative that India ensures they fight not only Covid-19, but also the other infectious diseases that plague the country, especially with the disruption of health care services and livelihoods of Indians, due to one of the most stringent lockdowns. While it picked up pace rather late after allowing the infection to spread, India has been testing aggressively lately, reaching 42,000 tests per million.
Bangladesh and Pakistan present similar scenarios, wherein Covid-19 infections have surpassed 300,000 and death per million population is 29 for both the countries. Both countries have been demonstrating a flattening trend in terms of cases as well as deaths, however, they have also shown a lower testing per million population—Pakistan (13,510 tests per million) and Bangladesh (10,645 tests per million)—which could be one of the possible reasons for the lower number of cases. Similarly, Afghanistan has as low as 38,772 confirmed cases and 1,425 confirmed deaths, as of September 15th, but Afghanistan has one of the world’s lowest testing statistics, with a total of 107,167 tests conducted, which make up 2,740 tests per one million population. The low level of tests and the subsequent fall in the cases has raised questions regarding the reliability and transparency in the data being shared.
The trajectory of Nepal and Sri Lanka has been completely different. Nepal has observed a lower number of cases as well as fatalities from the beginning, while maintaining strong testing capabilities, but the month of September has seen a surge in cases. The surge in cases has raised some concerns, but at just 12 COVID-19 deaths per million, the mortality burden is low, and the government seem confident that the spread can be effectively contained. Amongst the South Asian countries, Sri Lanka has the lowest levels of infection (152 cases per million population), with only 13 recorded Covid-19 deaths so far. The country has been applauded for its strict quarantine rules and robust contact tracing, effectively curbing the spread of the disease.
Termed as the ‘Coronavirus Success Story’, Bhutan has been successfully detecting and containing the spread of the disease by strongly imposing quarantine on returning international citizens, and deployment of tech-based solutions to enhance contact tracing. Bhutan has also borne the cost associated with testing, quarantine and treatment, in addition to providing financial assistance to its citizens to ease the pandemic stress. With only 246 cases and no deaths, Bhutan has devised an effective prevention and control system.
In the global comparison sheet, South Asia’s performance has been more or less positive, but with no vaccination in the picture, these countries must remain vigilant. South Asia also constitutes a large conflict-affected population, in addition to a considerable poor and highly immune-compromised population, making it extremely volatile to the future events. It was recently suggested by an industry leader that at least four to five years will be needed to provide vaccinations to the global population.
Moreover, multiple barriers still need to be overcome to determine whether the emerging vaccine will be able to effectively reach the masses. Given the high population densities and low income in the South Asian countries, a vaccine may not present the perfect solution. Past experiences have taught us that lesser developed countries need to be prepared for delayed availability of the vaccine and therefore need to dedicate resources in to preventive measures; while at the same time re-starting their economies cautiously to maintain the levels of human development that have been achieved in the past decade, and to prevent a parallel human tragedy.
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.

Oommen C. Kurian is Senior Fellow and Head of Health Initiative at ORF. He studies Indias health sector reforms within the broad context of the ...
Read More +
Kriti Kapur was a Junior Fellow with ORFs Health Initiative in the Sustainable Development programme. Her research focuses on issues pertaining to sustainable development with ...
Read More +