-
CENTRES
Progammes & Centres
Location

When the Covid-19 pandemic struck India, one assumed that states with inadequate health systems, high disease burden and lower literacy rates may be worst affected, simply because they may not be able to cope with the necessary preventive measures such as maintaining social distance, wearing masks or washing hands. However, some states in India, particularly Bihar, have proven all such gloomy forecasts wrong.
Bihar is one of the eight Empowered Action Group (EAG) states, with a lower socioeconomic status, characterized by high levels of infant mortality, low levels of education and a slow demographic transition. Bihar has one of the lowest literacy rates in the country, and with an overall score of 32.11, it was ranked one of the lowest in the NITI Aayog Health Index.
Similarly, Bihar’s death per million population, of 9, is the amongst the lowest in the country.
However, Bihar’s lagging health infrastructure has seemingly not impacted its pandemic performance. As of October 26th, out of 212,192 confirmed cases, 200,920 had already recovered, while the death toll amounted to 1049. Bihar’s case per million population, at 1,775, has been considerably lower when compared to its equally populous counterparts, such as Maharashtra with 13,612 cases per million population. Similarly, Bihar’s death per million population, of 9, is the amongst the lowest in the country. During the pandemic, Bihar has emerged a ‘topper’ in terms of several parameters to measure the Covid-19 burden across India—with the lowest test positivity rate of 2.1 percent, along with one of the best case fatality rates of 0.05 percent and recovery rate of 94.7 percent.
But a critical question that needs to be raised is whether Bihar’s performance during the pandemic is a true indicator of the overall performance of its health system.
During a pandemic, key factors such as the historic disease burden, prevalence of illiteracy and malnutrition and the robustness of health systems and processes play a crucial role in preparedness and prevention.
The NITI Aayog Health Index report illustrates the deterioration of Bihar’s overall performance between 2015-16 and 2017-18, with a fall in many important indicators such as total fertility rate, low birth weight, sex ratio at birth, institutional delivery, TB notification rate, staff nurse vacancies and functional 24x7 PHCs. While most states saw an improving trend, Bihar saw a decline of 6.35 points from 2015-16 to 2017-18—the biggest fall in the health index amongst larger Indian states. Compared to other states, Bihar observed a negative performance in 16 indicators, the most amongst the larger states.
Figure 1: Health Index Progress (Large States)
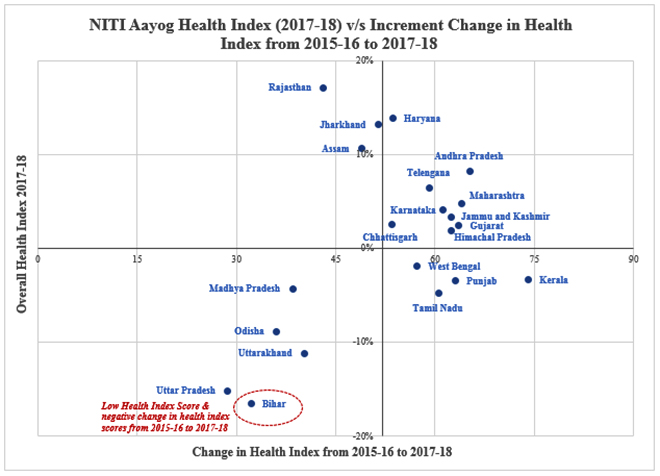 Source: Author’s Own, Data: NITI Aayog Health States, Progressive India
Source: Author’s Own, Data: NITI Aayog Health States, Progressive India
In 2016, as per the Bihar Disease Burden Profile, the leading causes of deaths and disability in Bihar were diarrhoeal diseases (7.6 percent), ischaemic heart disease (6.6 percent), lower respiratory infections (6.4 percent) and iron-deficiency anaemia (4.3 percent). In totality, communicable, maternal, neonatal and nutritional diseases contributed to 42.6 percent of the total disease burden in Bihar.
Figure 2: Causes of Deaths in Bihar, 2016
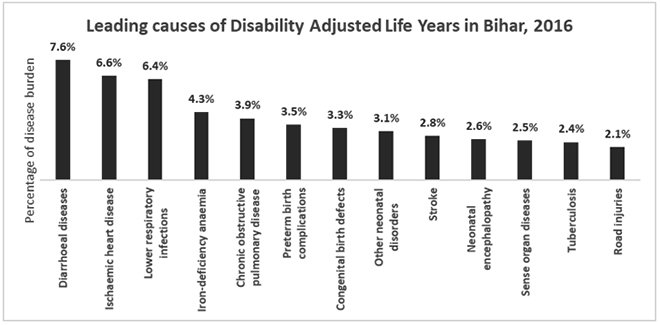 Source: Author’s Own, Data: Bihar: Disease Burden Profile, 1990 to 2016
Source: Author’s Own, Data: Bihar: Disease Burden Profile, 1990 to 2016
The age-wise breakup of the total deaths in Bihar shows that 38.2 percent of the deaths are contributed by people of 40-69 years, followed by 70+ years (31.6 percent), 0-14 years (18.6 percent) and 15-39 years (11.6 percent). For people aged 40 years and above cardiovascular diseases and chronic respiratory diseases contributed to more than 45 percent of the deaths.
Figure 3: Bihar’s Nutrition Status
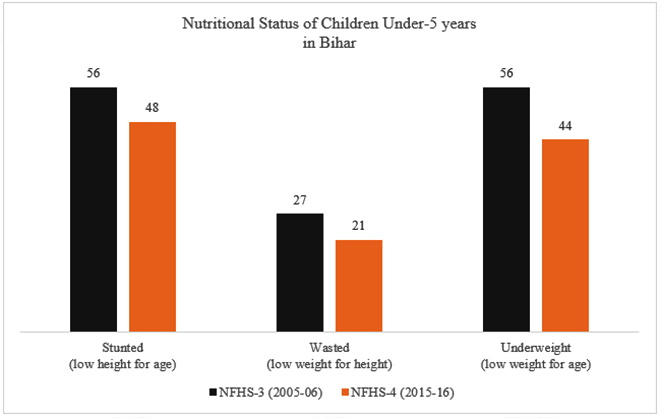 Source: NFHS 4 2015-16
Source: NFHS 4 2015-16
While observing the nutritional status of Bihar, we see immense improvement in the nutrition indicators since 2005-06, however the current scenario is far from satisfactory. An unacceptably high 48 percent of children under the age of five are stunted, whereas, 21 percent are wasted and 44 percent are underweight. Meanwhile, 42 percent of the women and 38 percent of the men are either overweight or obese or too thin. Programmes such as ICDS and POSHAN Abhiyaan have been effective in improving the necessary nutritional requirements of children and adults, however, gaps in the system continue to persist.
Figure 4: Integrated Child Development Service (ICDS) availability in Bihar (%)
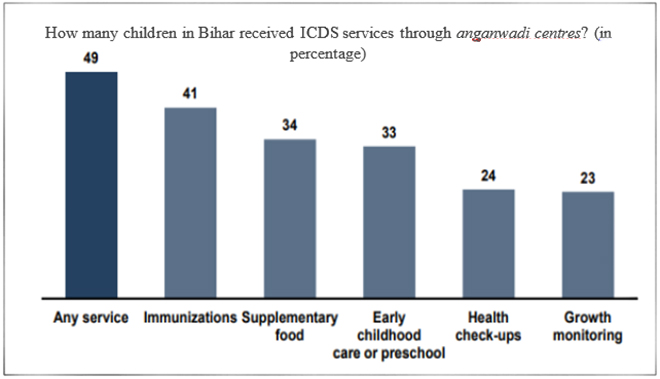 Source: NFHS 4 2015-16
Source: NFHS 4 2015-16
In terms of provision of health care and operational facilities, Bihar has a long way to go. Only one third of the women received any antenatal care during the first trimester of their pregnancy, with only 14 percent receiving the recommended 4+ antenatal care visits. Similarly, less that 62 percent of the children (below 2 years of age) receive all the basic vaccinations against major child hood diseases. On the other hand, 7 percent of the children received none of the designated vaccinations. Additionally, 60 percent women, 32 percent men and 64 percent children (6-59 months) in Bihar were characterised as anaemic—possibly leading to nutritional deficiencies, increased morbidity due to infectious diseases or chronic infections, diminished physical and mental capacity and weakened cognitive performance.
The heavy burden of disease and malnutrition in Bihar had led to fears that the state may become a hotspot. It was surprising to observe that the Covid-19 spread in Bihar started at a much later stage, but also the intensity of the spread was far lesser than expected from a state with a weak healthcare infrastructure.
While testing has increased in Bihar, only a small percentage of these tests are the ICMR recommended RTPCR Covid-19 tests.
At the onset of the pandemic, states and territories across India were working on increasing testing capacity, but Bihar started slow. As of May 11th, Bihar had one of the lowest testing capacities in the country, with 1,811 tests being conducted in a day, across 7 testing centres. Since then, Covid-19 testing centres in Bihar have risen to 48 government facilities and 13 private facilities, that have been conducting over ~100,000 tests a day since mid-August. The past week has observed the average testing rate to rise to ~140,000. While testing has increased in Bihar, only a small percentage of these tests are the ICMR recommended RTPCR Covid-19 tests. It was estimated that more than 93 percent of the test that were being conducted in Bihar were the rapid-antigen tests, known to have a 40 percent probability of false-negative results. However, numbers indicate that rapid tests have been a handy tool in the field to contain the spread, since the delay between sample collection and results was brought down substantially; leading to early detection, early isolation and early treatment.
Figure 5: Confirmed cases and Covid-19 tests in Bihar
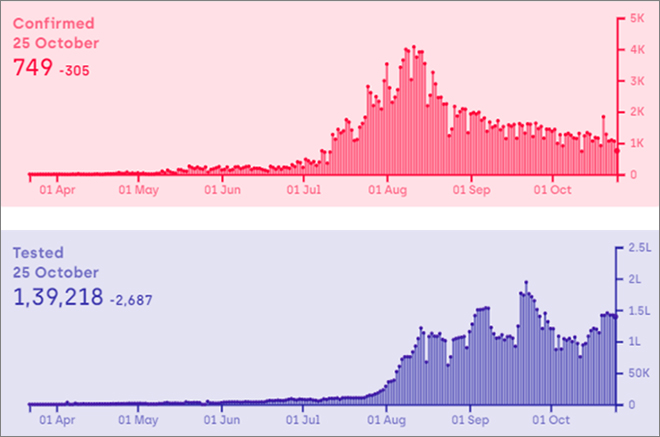 Source: Bihar state profile, Covid19India
Source: Bihar state profile, Covid19India
Bihar’s much applauded recovery ratio of 94.7 percent (as on Oct 26) has been widely used as a measure of the ruling government’s strong pandemic response, but one must note that the recovery rate could easily be a product of the mildly symptomatic or asymptomatic nature of the disease in the state with the largest concentration of Indians (58 percent) below the age of 25. Additionally, Bihar’s contact tracing mechanism has been very lenient—with people who tested positive being trusted to self-isolate and maintain social distancing, rather than being isolated in government monitored facilities. Recently, the Bihar government, in a first, promised free vaccination to all the citizens of the state as a part of the election manifesto—which seems to be a rather difficult task for a populous state considering the enormous logistical and distributional challenge associated with it.
Bihar’s pandemic prevention and testing strategy, coupled with the looming elections in the state, has raised questions on whether the government is lax in their pandemic response in view of the elections.
Bihar’s pandemic prevention and testing strategy, coupled with the looming elections in the state, has raised questions on whether the government is lax in their pandemic response in view of the elections. Reportedly, Covid-19 norms are being flouted regularly during election campaigns. Until now, Bihar has escaped the disturbing impact of the Covid-19 pandemic, but its overall health profile points towards an inadequate healthcare system and infrastructure, putting the state in the high-risk category.
Given the current scenario, Bihar must maintain the focus on improving the environmental and social conditions of its people to provide sound physical, mental and economic stability. Government initiatives like ‘Har Ghar Jal’ and ‘Har Ghar Bijli’ have increased the household penetration of tap water from 1.62 percent to 54.96 percent between 2019 and 2020, and ensured the provision of electricity across all villages of Bihar, respectively. The School Education Quality Index (SEQI) also shows the steady rise of equitable access to education and attendance in schools; on the other hand, ‘Ghar Tak Pakki Gali Naliyaan’ mission aims to deliver connectivity and drainage solutions to the rural wards of the state. While these initiatives present a good beginning, the state has a long way to go to ensure the health and wellbeing of its citizens.
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.

Kriti Kapur was a Junior Fellow with ORFs Health Initiative in the Sustainable Development programme. Her research focuses on issues pertaining to sustainable development with ...
Read More +