-
CENTRES
Progammes & Centres
Location

Haryax Pathak, “India’s COVID-19 Vaccination Campaign: A Marathon, Not a Sprint,” ORF Special Report No. 143, June 2021, Observer Research Foundation.
The first confirmed case of COVID-19 in India[1] was reported in the southern state of Kerala on 30 January 2020, of a 20-year-old female returning from Wuhan. Sixteen months later, the reported cumulative case count stands at 28.3 million.[2] Globally, India stands second only to the United States (US) in absolute numbers of cases. In proportion to India’s entire population, the cases comprise two percent. As of 3 June 2021, India has had over 300,000 deaths due to COVID-19,[3] the highest number in the world after the US and Brazil. In terms of deaths per million population, India’s number is 234.[4]
India officially launched its COVID-19 vaccination drive on 16 January 2021, with two approved vaccines – Covishield and Covaxin. As of 3 June 2021, as per reports from the Ministry of Health and Family Welfare (MoHFW),[5] India has administered just over 221 million vaccine doses. Of India’s 1.38 billion population, only 45.1 million have been fully vaccinated at the time of writing –about 3.26 percent of the total population. The US, for instance, has fully vaccinated 41 percent of its population.[6]
Analysts agree that a quick vaccine rollout is India’s only way through the pandemic.[7] On 30 May, the government informed the public that while a little more than 79 million doses of COVID-19 vaccine were available with the states in May, nearly 120 million doses will be made available in June.[8]
Other than the question of supply, however, there are issues that are critical to whether or not India will succeed in its vaccination campaign.
Myths and misinformation around vaccines circulating on both traditional and social media have had a significant impact on the global vaccination drive. Probably the greatest fears towards vaccination stem from the fact that the vaccines have been developed at a rapid pace and the mechanism of how these vaccines work is almost completely unknown to the general population.[9],[10]
The US is one example of how a specific policy and mechanism has been put in place for the rapid development of vaccines—called Operation Warp Speed,[11] which it launched in May 2020. Vaccines usually take years to be developed and undergo trials, and Operation Warp Speed aimed to reduce that length of time, without compromising on the due scientific process. Other countries soon also started accelerating their vaccine development and approval process. (See Table 1) As a result, today there are over 300 vaccines in development across the world, with some already having received approval for emergency use.[12]
Table 1. COVID-19 Accelerated Vaccine Development
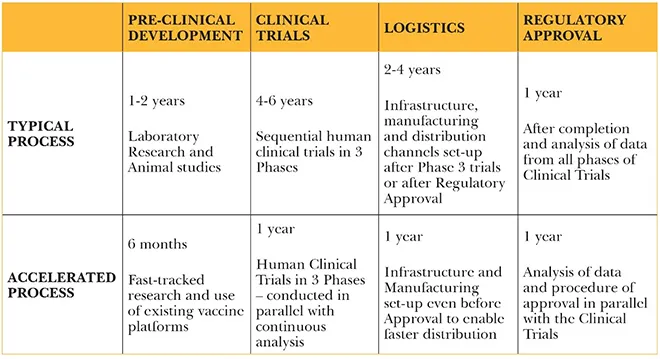
For India, the sheer magnitude of its 1.38-billion population makes it difficult to execute a swift rollout. Recognising the need for more vaccines to match the demand and the rising case count, the Drugs Controller General of India (DCGI)[14] made the decision to approve for use in the country all the vaccines being administered to different populations globally—as listed in the World Health Organization’s (WHO) Emergency Use Listing, or approved by organisations like the United States Food and Drug Administration (USFDA), the European Medicines Agency (EMA), the United Kingdom Medicines and Healthcare products Regulatory Agency (UK MHRA), and the Pharmaceuticals and Medical Devices Agency, Japan (PMDA Japan).
Table 2. Development and Manufacture of Vaccines in India
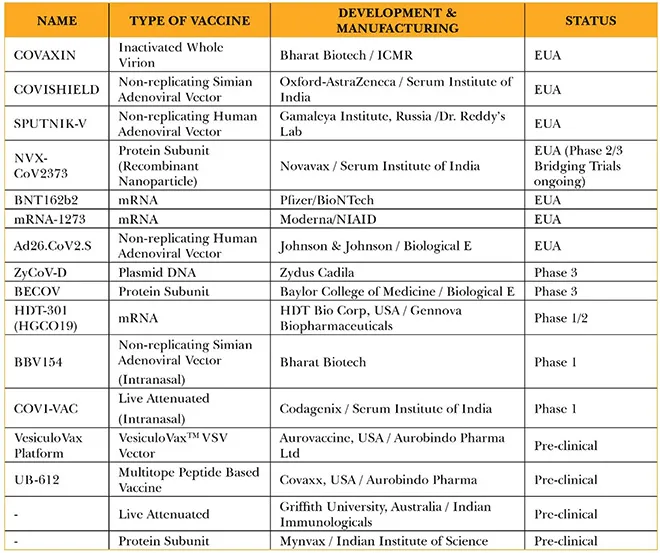
Sputnik-V—manufactured and distributed in India by Dr. Reddy’s Lab—is the third vaccine after Covishield and Covaxin to receive Emergency Use Approval in India. Meanwhile, the MatrixMTM protein subunit vaccine platform[a] from Novavax has shown promising results[18] against the variants and is undergoing Phase II/III bridging trials[b] in the country, in collaboration with the Serum Institute of India. For their part, the mRNA vaccines[c] from Pfizer and Moderna are expected to receive emergency use approval in the near future as negotiations are ongoing between the companies and the Government of India. They are expected to be important vaccines in the Indian context as they have shown some measure of efficacy against the B.1617,[19], [20], [21] B.1.1.7, and the B1.135[22] variants. Gennova Biopharmaceuticals is also developing a vaccine, HGCO19, based on a similar mRNA platform.
The BBV154 intranasal vaccine from Bharat Biotech is another vaccine candidate in development. Being intranasal, it is expected to induce mucosal immunity which should prevent infection and transmission of the virus as well. COVI-VAC, another intranasal vaccine from Codagenix, should also be crucial in reducing the transmission.
While India has reached a notable number of individuals for its vaccine rollout in a short time of five months, it is nowhere near enough to have an impact on the overall targets for herd immunity. India’s primary healthcare setup has the capacity to vaccinate five to 10 million people per day. However, there has been a palpable degree of vaccine hesitancy, coupled with difficulties in using the online Co-WIN portal for securing slots for appointment, a shortage in doses, and wastage.
Across the globe, there are sections of people who have historically denied the need for vaccines. These people—referred to as “vaccine denialists”—launch vocal, active public campaigns against the use of any vaccine, including the ones for COVID-19. Their protests against the use of vaccines find space in both mainstream and new media, and reach significant numbers of people.
Another aspect of vaccine hesitancy is related fundamentally to fear. As vaccines are biological agents, they are bound to have side effects, differing in form and degree between individuals. The perception of the side effects of the COVID-19 vaccines has become exaggerated. Rarely, adverse events, allergies, anaphylactic reactions, or some other life-threatening events may occur post-vaccination, owing to multiple factors other than the vaccines themselves. But even rare events, like the post-vaccination clotting incidents in Europe,[23] are enough to create massive doubt in the minds of the potential recipients.
India must engage in proactive measures to address and dispel hesitancy and gain trust for vaccination.
A successful story comes from the remote village of Janefal,[24] in Aurangabad, Maharashtra, where the authorities have managed to vaccinate 100 percent of the eligible population through constant health messaging, awareness campaigns, and confidence-building measures. Indeed, effective vaccination coverage and uptake in rural areas requires a bottom-up approach: developing infrastructure at the ground level and mobilising human resources like grassroots health workers and volunteers to disseminate proper and adequate information to rural families who might be initially hesitant to get themselves vaccinated.
To streamline the process of vaccination, the Indian government developed a digital platform – called Co-WIN – where one could book an appointment for vaccination, check the status of vaccination, and later download their vaccination certificate. The same portal allows the government to keep track of the country’s vaccination statistics. The idea was simple enough: digitise the process, avoid the hassles of analog record-keeping, and allow for easy data management. However, Co-WIN has had its fair share of problems.
As India opened up Phase 2 of its vaccination campaign in March for the elderly and those with comorbidities, the portal was flooded with millions of users trying to book a slot. The surge resulted in glitches in the mobile application or the website, with servers going down and users unable to find and block an appointment. Even as medical staff are required to undergo training in using the web portal, errors have been reported in data entry – either from the recipients or the authorities – that has led to duplication or erasure of many details. The flaws were heightened as vaccination opened up, first, for everyone above 45 including those without comorbidities, and later for those above the age of 18. The portal was overloaded, and there was a shortage of slots available for those who logged in.
While Co-WIN was meant to facilitate the vaccination drive, it needs more logistical support in terms of ease of access and use. The past few weeks have revealed the system’s weaknesses, especially for use in the rural regions, as pointed out by the Supreme Court of India in a recent directive.[25]
Wastage is a common enough issue for any vaccination drive of a similar scale as what India is attempting. There are various reasons,[26] primary of which are improper cold-chain maintenance and poor vaccine administration practices like inability to draw the stipulated number of doses from a vial. The concern with COVID-19 vaccines, however, is the amount of wastage occurring in India. Wastage creates an unnecessarily high demand for vaccines, while also slowing down the entire campaign.
Wastage of both Covishield and Covaxin has been brought down drastically over the past two months to under five percent as of 22 May 2021. The national average, as of 25 May 2021,[27] is 6.5 percent, with many states reporting wastage levels of over 30 percent. Consistent efforts are needed to keep this wastage to a minimum.
The key to curbing the COVID-19 pandemic is widespread vaccination, at a rapid pace, among the populations in rich and poor countries alike. The aim is vaccine equity. The Lower Middle Income Countries (LMIC), with their limited technology and resources, are dependent on the global vaccine alliances of WHO, the United Nations, The Gates Foundation, as well as GAVI and COVAX—where the wealthy regions have pledged to supply vaccines to the poorer nations. As seen in Figure 1, while the large economies have vaccinated a majority of their populations, the pace in the poorer nations has been painfully slow.
Figure 1. COVID-19 Vaccination by Country Income Group

At the same time, India, as part of its ‘Vaccine Maitri’ initiative, has sent vaccines to many poor nations across the globe. As of 28 May, India has sent over 66.37 million doses[29] of both Covishield and Covaxin, to 95 countries. Amidst growing concerns that the effort is resulting in domestic shortages, the government and the Ministry of External Affairs[30] have maintained that the vaccine diplomacy has not compromised the country’s own need.
In October 2020, India and South Africa moved the World Trade Organization (WTO) to waive certain provisions of the agreement on Trade-Related Aspects of Intellectual Property Rights (TRIPS).[31] The aim of this plea was to encourage data-sharing and the necessary technology transfer, thus enabling the low-income nations to manufacture the mRNA vaccines and drugs for wider distribution and faster treatment/vaccination of their populations.
While the plea received a largely negative response initially, seven months later, the US has given its conditional approval[32] of the proposal. Following this, even the European Union,[33] New Zealand,[34] and France[35] have shown willingness to negotiate the terms and conditions of the TRIPS waiver.
As large and diverse India is, vaccine equity is a challenge within the country as well. During the first wave of the pandemic, the rural areas were relatively less affected compared to the urban regions. Eventually, the rural regions saw a significant surge in cases, especially in the second wave. An analysis conducted by the State Bank of India[36] states that the share of rural districts in COVID-19 cases is 52.9 percent as of May 2021. Even in the first wave, the peak was at 53.7 percent of cases. It is a worrying trend, as rural areas also see lower rates of testing and poor reporting.[37]
The primary reason for this urban-rural divide is logistical constraints—infrastructure, supply chain, and skilled personnel, especially in the poorer states.[38] For the vaccination drive to be effective, the poorer states need resources and capacity building to improve the health infrastructure, which includes a very important component – i.e., Cold Chain.[d] While the vaccines in use currently do not have extreme cold chain requirements, the nationwide distribution of cold chain points in India is uneven. As of December 2020, India has 29,000 cold chain points across the country.[39] A detailed analysis by the IDFC Institute[40] in March 2021 reveals that six states with 34 percent of India’s population have 52 percent of the entire country’s cold chain points (See Figure 2).
Figure 2. No. of Cold Chain Points and Equipment Across India, by State
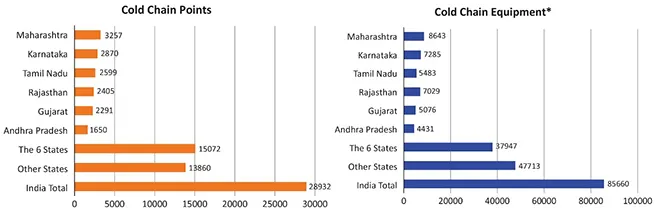
The vaccination of an individual may seem straightforward—like a 100m sprint. Mass inoculation, however, is more of a 10,000m marathon and obstacle run, with hurdles erected in various points and manifesting in myriad forms. India will need a multipronged approach to tackle these hurdles. At the time of writing this report, the second wave was on the downward trend; the third wave is expected around November– this interval must be used as a buffer to launch the vaccination campaign into overdrive.
This report offers the following recommendations.
Haryax Pathak is a medical doctor from Vadodara.
[a] Protein Subunit Vaccine – The antigenic proteins of the virus – the Spike Protein in this case – are developed outside the human body, in a lab, and then delivered to the human body as a vaccine.
[b] Bridging trials are small-scale clinical trials conducted in a new region/population to extrapolate the efficacy, safety and immunogenicity data from the large-scale clinical trials conducted in a foreign population.
[c] mRNA is a piece of genetic code responsible for protein synthesis in the human body. The genes coding for the Spike protein are encoded onto an mRNA segment. This mRNA vaccine delivers the code to the human cells that eventually express the Spike protein on their surface.
[d] Cold Chain is a temperature-controlled supply chain network of cold-chain points comprising of cold rooms, walk-in coolers, ice-lined refrigerators, deep freezers, vaccine carriers and solar units. This cold-chain is necessary to maintain the viability of the vaccine during transportation and storage – as per the given temperature requirements.
[1] Andrews, M. A., Binu Areekal, K. R. Rajesh, Jijith Krishnan, R. Suryakala, Biju Krishnan, C. P. Muraly, and P. V. Santhosh. 2020. “First Confirmed Case of COVID-19 Infection in India: A Case Report”. The Indian journal of medical research 151 (5): 490–92.
[2] Ministry of Health and Family Welfare, “COVID-19 Statewise Status”.
[3] Ministry of Health and Family Welfare, “COVID-19 Status”.
[4] Worldometer, “COVID-19 Coronavirus Pandemic”.
[5] Ministry of Health and Family Welfare, “Cumulative Covid Vaccination Report 2nd June 2021”.
[6] Centers for Disease Control and Prevention, “COVID-19 Vaccinations in the United States”.
[7] Rakesh Sood, Kriti Kapur and Oommen C Kurian, “India’s Vaccine Rollout: A Reality Check,” ORF Special Report No. 139, May 2021, Observer Research Foundation.
[8] Government of India, “Update on COVID Vaccine Allocation“, Press Information Bureau, May 30, 2021.
[9] Loomba, Sahil; Figueiredo, Alexandre de; Piatek, Simon J.; Graaf, Kristen de; Larson, Heidi J. (2021): Measuring the impact of COVID-19 vaccine misinformation on vaccination intent in the UK and USA. In Nature human behaviour 5 (3), pp. 337–348. DOI:
[10] Islam, Md Saiful; Kamal, Abu-Hena Mostofa; Kabir, Alamgir; Southern, Dorothy L.; Khan, Sazzad Hossain; Hasan, S. M. Murshid et al. (2021): COVID-19 vaccine rumors and conspiracy theories: The need for cognitive inoculation against misinformation to improve vaccine adherence. In PloS one 16 (5), e0251605.
[11] United States Department of Defense, “Coronavirus: Operation Warp Speed”.
[12] COVID-19 Vaccine Tracker.
[13] World Health Organisation (2020): Update on COVID-19 Vaccine Development. Available online at, updated on 12/21/2020
[14] Directorate General of Health Services (2021). Central Drugs Standard Control Organisation.
[15] World Health Organisation (2021): Draft landscape and tracker of COVID-19 candidate vaccines.
[16] Jeff Craven (2021): COVID-19 vaccine tracker. Regulatory Affairs Professionals Society (RAPS). updated on 5/27/2021
[17] Sharun, Khan; Dhama, Kuldeep (2021): India’s role in COVID-19 vaccine diplomacy. In Journal of travel medicine.
[18] Shinde, Vivek; Bhikha, Sutika; Hoosain, Zaheer; Archary, Moherndran; Bhorat, Qasim; Fairlie, Lee et al. (2021): Efficacy of NVX-CoV2373 Covid-19 Vaccine against the B.1.351 Variant. In The New England journal of medicine 384 (20), pp. 1899–1909.
[19] Planas, Delphine; Veyer, David; Baidaliuk, Artem; Staropoli, Isabelle; Guivel-Benhassine, Florence; Rajah, Maaran Michael et al. (2021): Reduced sensitivity of infectious SARS-CoV-2 variant B.1.617.2 to monoclonal antibodies and sera from convalescent and vaccinated individuals. In bioRxiv : the preprint server for biology.
[20] Tada, Takuya; Zhou, Hao; Dcosta, Belinda M.; Samanovic, Marie I.; Mulligan, Mark J.; Landau, Nathaniel R. (2021): The Spike Proteins of SARS-CoV-2 B.1.617 and B.1.618 Variants Identified in India Provide Partial Resistance to Vaccine-elicited and Therapeutic Monoclonal Antibodies. In bioRxiv : the preprint server for biology.
[21] Edara, Venkata-Viswanadh; Lai, Lilin; Sahoo, Malaya K.; Floyd, Katharine; Sibai, Mamdouh; Solis, Daniel et al. (2021): Infection and vaccine-induced neutralizing antibody responses to the SARS-CoV-2 B.1.617.1 variant. In bioRxiv : the preprint server for biology.
[22] Abu-Raddad, Laith J.; Chemaitelly, Hiam; Butt, Adeel A. (2021): Effectiveness of the BNT162b2 Covid-19 Vaccine against the B.1.1.7 and B.1.351 Variants. In The New England journal of medicine.
[23] Cines, Douglas B.; Bussel, James B. (2021): SARS-CoV-2 Vaccine-Induced Immune Thrombotic Thrombocytopenia. In The New England journal of medicine.
[24] Puja Changoiwala (2021): How a village in India reached 100% vaccination in the face of misinformation and hesitancy. National Geographic. Updated on 5/22/2021
[25] Supreme Court of India, of 5/31/2021, Suo Motu Writ Petition (Civil) No.3 of 2021 IN RE: DISTRIBUTION OF ESSENTIAL SUPPLIES AND SERVICES DURING PANDEMIC, pp. 27–31. E.5.
[26] Ministry of Health and Family Welfare, “Vaccine Wastage Assessment”, April 2010.
[27] Ministry of Health and Family Welfare, 25 May 2021.
[28] Mathieu, Edouard; Ritchie, Hannah; Ortiz-Ospina, Esteban; Roser, Max; Hasell, Joe; Appel, Cameron et al. (2021): A global database of COVID-19 vaccinations. In Nature human behaviour.
[29] Ministry of External Affairs, COVID-19 Vaccine Supply, “Vaccine Maitri”.
[30] Ministry of External Affairs, “Statement by External Affairs Minister in Lok Sabha on the Vaccine Maitri Initiative”, 17 March 2021.
[31]World Trade Organization: “Waiver From Certain Provisions Of The Trips Agreement For The Prevention, Containment And Treatment Of Covid-19”.
[32] Office of the United States Trade Representative, “Statement from Ambassador Katherine Tai on the Covid-19 Trips Waiver.” Washington. 5 May 2021.
[33] European Union, “Statement by President von der Leyen at the joint press conference with President Michel and Prime Minister Costa following the informal meeting of EU Leaders and the EU-India leaders’ meeting.” 8 May 2021.
[34] New Zealand, “NZ backs moves to improve global access to COVID vaccines.” 6 May 2021.
[35] Macron backs waiving IP rights for COVID-19 vaccines. Reuters. 6 May 2021.
[36] State Bank of India (2021): INDIAN STATES & GLOBAL VACCINATION MARKET: THE TEMPLATE FOR MAKING STATE VACCINE PROCUREMENT A SUCCESS. Issue no. 12, FY22 (Ecowrap).
[37] Vignesh Radhakrishnan: Vaccination in rural India trails urban areas even as cases surge. The Hindu.
[38] Ministry of Health and Family Welfare, “Rural Health Statistics”, 2018-19.
[39] Ministry of Health and Family Welfare, 25 December 2020.
[40] The Indian COVID-19 Alliance (2021): India COVID-19 Vaccination Distribution Report. IDFC Institute.
[41] World Health Organisation: WHO Policy Statement: Multi-dose Vial Policy (MDVP). 2014.
[42] Sangeeta Ojha, “Drive-in Covid-19 vaccinations centres in these cities in India. Full list.” Mint. 18 May 2021.
[43] PTI “Drive-through COVID-19 vaccination centre starts in Ahmedabad.” 27 May 2021.
[44] PTI, “Kolkata to Get Its First Drive-through Vaccination Centre.” News 18 India. 2 June 2021.
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.

Dr Haryax Pathak is a doctor from Vadodara. He is a hobbyist photographer and writer and an advocate for Creative Pedagogical Practices. His other interests ...
Read More +