-
CENTRES
Progammes & Centres
Location
 PDF Download
PDF Download 
Oommen C. Kurian is a Fellow at Observer Research Foundation, New Delhi. He wishes to thank an anonymous referee for helpful inputs on an early draft of this paper.
Introduction
Formed in 1997, the Bay of Bengal Initiative for Multi-Sectoral Technical and Economic Cooperation (BIMSTEC) is a group of countries from South Asia and South East Asia: Bangladesh, India, Myanmar, Sri Lanka, Thailand, Bhutan and Nepal. Most of these countries are known to have low levels of health and nutrition, part of what has come to be known as the ‘Asian Enigma’ of undernutrition. In these countries, underweight rates are substantially higher than in most sub-Saharan African countries, despite having similar or better income levels.[1]
BIMSTEC originated from an amalgamation of India’s ‘Look East Policy’ (now ‘Act East Policy’) and Thailand’s ‘Look West Policy’.[2] The BIMSTEC group of countries have identified 14 priority areas for cooperation, with public health being one of them. Thailand leads the public health theme within BIMSTEC. The joint statement of the 15th BIMSTEC Ministerial Meeting held in Kathmandu in 2017 recognised the importance of holistic public healthcare among the BIMSTEC member states and the need to establish alliances.[3] Historically, most intra-BIMSTEC collaborations have been around traditional medicine, which only under seven percent of the Indian population currently uses to treat diseases, making its scope rather narrow.[4] However, the launch of the JIPMER- BIMSTEC Telemedicine Network (JBTN) by the Jawaharlal Institute of Postgraduate Medical Education and Research India in July 2017—designed to strengthen links among premier medical institutions in the region—has expanded the collaborations into modern medicine as well.[5]
The JBTN initiative combines public health, communication, and technology: three of the 14 stated areas of cooperation among BIMSTEC countries. Spearheaded by India, this initiative receives financial and technical support from the Government of India.[6] At the launch stage, the network intends to connect nine healthcare institutions across seven BIMSTEC countries. Eventually, the initiative plans to establish state-of-the-art facilities for multi-organ transplantation, transplant medicine and post-transplant care of patients.[7]
All BIMSTEC countries are categorised as either low- or middle-income; Thailand is the richest and only upper-middle income country in the group. The leadership role India plays within BIMSTEC is not a result of its average income levels: Thailand, Sri Lanka and Bhutan have had a higher per capita gross domestic product (GDP) than India for the last two-and-a-half decades (see Figure 1). There is no factual basis for recent assertions that Bhutan’s per capita income was half of India’s 20 years ago and is now twice that of India’s only because of the profits from trade in hydel power with India.[8] Bhutan has had a higher per capita GDP than India as far back as 1980.[9]
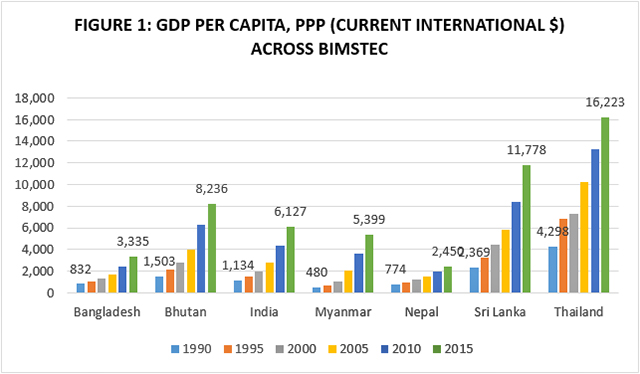
The rest of this brief will offer a comparative look at the health status and trends of BIMSTEC countries, and seek out lessons for India’s health sector. For want of internationally comparable data, the analysis is limited mostly to data from 1990 to 2015, also known as the Millennium Development Goals (MDG) era.
Health Indicators within BIMSTEC Countries
From 1990 onwards, while India has maintained its fourth rank in terms of per capita GDP within BIMSTEC, and improved its income faster than poorer countries such as Bangladesh and Nepal, the income gains have not been reflected in its social indicators. As Jean Dreze and Amartya Sen note, comparing social indicators between India and Bangladesh, “The history of world development offers few other examples, if any, of an economy growing so fast for so long with such limited results in terms of reducing human deprivations.”[10]
Health is a case in point. As Figure 2 shows, many BIMSTEC countries have overtaken India in terms of child mortality reduction over the last few decades. In 1990, Nepal, Bangladesh and Bhutan had under-five mortality rates much worse than India did, but they are now doing much better. In terms of child mortality, India was fourth out of seven BIMSTEC countries in 1990, and in 2015, it was sixth. In terms of maternal mortality reduction too, the achievements of these countries over the last two decades are exemplary (see Figure 3), often at per capita health expenditure levels much lower than India’s (see Figure 4).
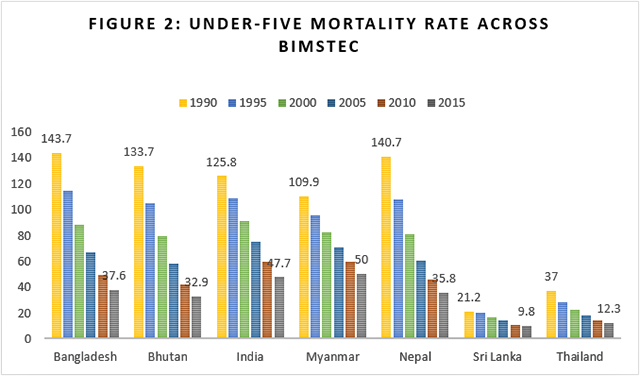
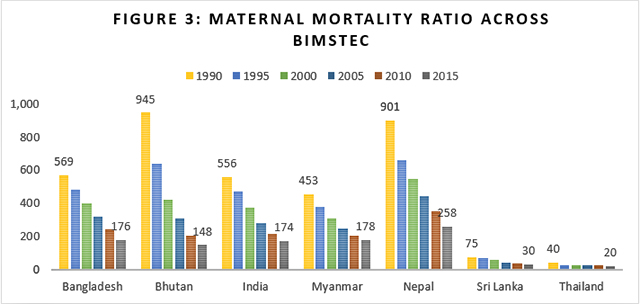
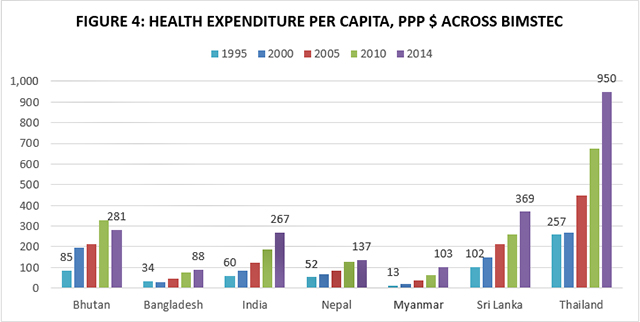
Figure 4 shows that, in terms of overall per capita health spending, India does not do too badly even when compared to richer countries such as Sri Lanka or Bhutan. It has increased the fastest among all BIMSTEC countries. What then is the explanation for India’s less-than-satisfactory performance in health? Part of the reason, according to Dreze and Sen (2013), are the stark inequalities that make India “look more and more like islands of California in a sea of sub-Saharan Africa” whereby, on the average, the country is “climbing up the ladder of per capita income while slipping down the slope of social indicators.”[11]
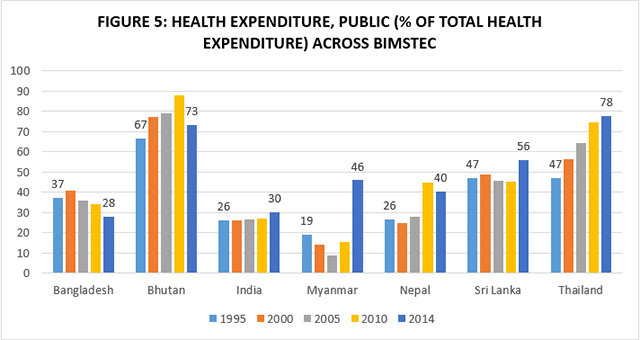
Another reason may be the extremely low public spending on health as shown in Figure 5. India ranks fourth in terms of total health spending, but is second last in terms of public spending as a percentage of total spending among BIMSTEC partners. This results in high levels of out-of-pocket spending, high levels of indebtedness, and a great number of households being forced to forgo care. Due to such factors, those who need health and allied services the most are less likely to access them. It is true that Bangladesh’s per capita health spending and percentage government spending are worse than India’s. However, experts point out that much of its rapid progress in social indicators has been because of the agency of women, girls’ education, and the involvement of women in the expansion of public services as well as in the industrial labour force.[12]
India’s lacklustre performance in health within BIMSTEC is despite its being one of the best among the member countries in terms of health workforce availability. India’s density of skilled health professionals is above the global threshold recommended by the World Health Organization (WHO) to deliver essential health services for the population, which is 22.8 per 10,000 (see Figure 6).[13] India has 24.1 skilled health professionals per 10,000 people, while Thailand has 25.6—only marginally higher—despite being a substantially richer country with universal health coverage (UHC) for its population.[14]

However, rural–urban disparities in workforce availability in India, as well as the predominance of private healthcare, prevents the high availability from translating into health system improvements. The Indian health workforce—barring the government funded frontline workers—are predominantly concentrated in tertiary and secondary healthcare institutions in urban areas where populations have the capacity to pay.[15] Innovative use of frontline workers in Bangladesh, Sri Lanka and Thailand has contributed to a revival of the primary-level care and helped consolidate health system achievements.
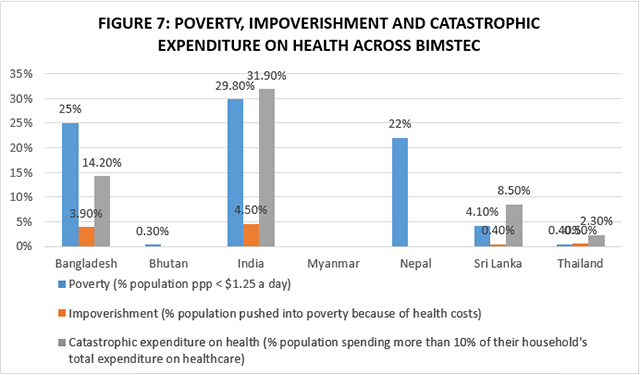
India’s poverty has a bidirectional relationship with its population’s health status. If one is poor, it is difficult to access quality health services. On the other hand, the process of accessing health services itself can render one considerably poorer, and often push them under the poverty line. As Figure 7 shows, among BIMSTEC countries for which data is available, India has the highest levels of poverty, highest levels of health-related impoverishment, and the highest proportion of population reporting catastrophic expenditure on health. India has a lot to learn from the experiences of its BIMSTEC partners—both richer and poorer—on how to keep health-related impoverishment and catastrophic expenditure under control.[16]
There is much to be learnt from Thailand’s case, which officially made Universal Health Coverage (UHC) a goal in 2002, when the economy was still reeling under the impact of the Asian financial crisis and its GDP per capita was at its lowest level in a decade.[17] Sri Lanka, meanwhile, represents an international case study for its health system, which offers healthcare at low cost. Even more remarkably, Bangladesh and Nepal have managed considerable improvements in health status at a fraction of the overall health expenditure of Sri Lanka or India (see Figures 3 and 4), even though they still have relatively high out-of-pocket spending.[18]
The following sections will examine the BIMSTEC states’ health-sector experiences over the MDG era, and identify the main drivers of health improvements and the potential lessons for India.
Bhutan
Among the richer countries within BIMSTEC, Bhutan has a Constitution that recognises free health services as a state responsibility, and government funds are the predominant source of health spending. Like India’s healthcare delivery system, Bhutan’s has a three-tier structure, with primary, secondary and tertiary levels, and often an integrated set of traditional and allopathic medicine services co-exist. Village-level health workers act as a bridge between government health services and the community, promoting and delivering basic services.[19]
Bhutan used to perform relatively low in terms of health indicators, despite being richer than most other BIMSTEC countries, barring Thailand and Sri Lanka. In 1990, it had higher child mortality figures than India, and a maternal mortality ratio that was almost double that of India. However, with focused government interventions, Bhutan now has better child as well as maternal health than India.
Beyond reproductive and child health, Bhutan has taken initiatives in the realm of non-communicable diseases (NCDs) as well. Bhutan happens to be one of the three countries in BIMSTEC—others being Sri Lanka and Thailand—that work closely with the Strategic Approach to International Chemicals Management (SAICM), an international policy framework to encourage sound management of hazardous chemicals, with the aim of strengthening the country’s capacity to manage industrial carcinogens such as asbestos. Given the potentially huge risk of asbestos-related diseases in India, firm steps in this direction are needed.
Thailand
Across the BIMSTEC countries, there has been tremendous progress in the collection and dissemination of health information over the last decades. However, availability of information does not necessarily lead to accountability. As the Thailand experience shows, the parliament, regional assemblies, civil society, and the public can together play an active role in the oversight mechanism within the health sector. The Thai National Health Assembly is a mechanism that facilitates multistakeholder engagement to ensure accountability.[20]
Thailand has a high NCD burden, as well as a very high road-traffic mortality rate: the highest among BIMSTEC countries. Almost all health facilities in Thailand have a steady supply of essential drugs and commodities.[21] The health volunteers in Thailand are a well-known example of government efforts to strengthen community-based health personnel, like the ASHAs (India’s Accredited Social Health Activists) in India (see Box 1).
Box 1: Village Health Volunteer Scheme in ThailandThe proposal for a Village Health Volunteer (VHV) force to provide basic healthcare for every village in Thailand was first made some 30 years ago. At first, it seemed impossible. How could volunteers be recruited from every single village in the country? With a desired critical ratio of 1:100—1 volunteer for every 100 people—the force would have to number in the hundreds of thousands to cover the whole country. Thirty years later, Thailand has a world-renowned VHV scheme. It has over 800,000 members today, serving a population of 65 million. From humble beginnings of giving simple care for diseases and injuries in the village, their role has expanded to cover other essential primary healthcare work such as water and sanitation, nutrition, and maternal and child health. The volunteers have also played key roles in the surveillance and control of communicable diseases such as HIV/AIDS, tuberculosis (TB) and avian influenza. And yes, they have been doing all of this for no pay. This is possible because voluntarism has deep cultural roots in Thailand. |
Source: http://apps.who.int/iris/handle/10665/204724.
The effort to revitalise primary healthcare was at the heart of Thailand’s progress to UHC. Going beyond medical care, a comprehensive community development approach was tried in Thailand under the title “Strategic Route Map (SRM),” a tool that facilitated community participation and empowerment.[22] Thailand’s move towards UHC—financed through multiple contributory pools, and substantial and focused government funding in a time of great economic distress—is now a global case study and is covered in another ORF publication written by key Thai health bureaucrats in charge of the transition.[23]
Nepal
Despite having only about one-third of India’s per capita GDP, Nepal has managed to overtake India in the reduction of child mortality and maternal mortality rates.[24] The efforts of the Female Community Health Volunteers in Nepal, who have similar work responsibilities as ASHAs, have been instrumental in Nepal’s stellar health achievements, despite the low level of overall health spending. There are other interesting parallels with India too: a scheme similar to India’s JSY exists in Nepal (see Box 2).
Box 2: Encouraging the Use of Skilled Birth Attendants in NepalNepal’s Safe Delivery Incentive Programme encourages greater use of professional care during childbirth. It provides cash transfers to women giving birth to offset their travel costs and an incentive to the health provider for each delivery attended, either at home or in the facility. The Government of Nepal recently launched the “Aama Surakchhya Programme,” which combines free delivery services at any public health facility with the Safe Delivery Incentive Programme. After the expansion of the Aama Programme to health posts and sub-health posts, marginalised ethnic groups are availing the services of skilled birth attendants and using emergency obstetric care much more now than they did previously. |
Source: http://apps.who.int/iris/handle/10665/204724.
Improvements in the coverage of effective healthcare interventions in Nepal to prevent or treat the most important causes of child mortality were brought about through a variety of community-based and centrally led approaches.[25] Nepal can offer solutions on what can be done even in an environment of turmoil and meagre resources, particularly to Indian regions where political unrest, poverty and breakdown of health services co-exist. Nepal received two awards for its efforts to contain maternal deaths: in 2010 by the MDG Review Summit and the 2012 Resolve Award.[26]
Like Bangladesh, Nepal’s efforts at extending the provision of safe abortion services to mid-level providers has contributed to bringing down maternal deaths considerably. In parallel, Nepal is working with international partners to develop an integrated “cause of death and birth” reporting system for hospital- and community-based data collection.[27] Nepal also managed to be polio-free before India.[28]
In tackling drug-resistant TB, Nepal provides a unique example of public–private partnerships, something India is now exploring. According to WHO, nearly half of the TB treatment centres in Nepal operate through partners, which include public and private hospitals and international NGO clinics, while an NGO partner GENETUP (German Nepal Tuberculosis Project) provides the services of a national reference laboratory.[29]
In light of the Gorakhpur incident, India’s high-burden areas of Japanese Encephalitis can learn from the experience of Nepal, which—despite a huge burden—chartered upon a mass vaccination campaign and managed to control the explosive outbreaks considerably.
Nepal also raises funds from the sale of alcohol and tobacco products and uses such funds for the free treatment of NCDs for the poor. Along with the private-sector engagement for treatment of NCDs that India is contemplating, such innovative financing methods may also be used to strengthen the overall strategy.
Bangladesh
Surprisingly, Bangladesh was one of the first within BIMSTEC partners—along with Thailand, a much richer country—to first achieve the MDG 4 target, which called for reducing the under-five mortality rate by two-thirds, between 1990 and 2015.[30]
Community health workers and volunteers played a key role in the country’s health achievements from the 1990s through the community clinics run across the country. To expand the supply of trained personnel, Bangladesh initiated two midwifery courses: six-month long and a three-year long. Bangladesh also provides vouchers to eligible women—based on poverty and vulnerability—to access maternal health services for three antenatal care visits, delivery, and one postnatal care visit by designated providers.[31] In 2010, Bangladesh announced that one-third of the maternal and child health clinics in the country will be transformed into adolescent-friendly clinics.
Bangladesh’s efforts at expanding the provision of safe abortion services to mid-level providers has resulted in reducing maternal deaths. The country also has an impressive track record of managing TB by successfully engaging with NGOs. Its menstrual regulation programme in the very early stages of pregnancy can offer India lessons on how culturally sensitive issues should be handled within health policy.
A radical transformation of Bangladesh’s routine health information system (HIS) has received policy attention.[32] Quite like India’s situation, assessments note that reflecting the country’s pluralistic health service delivery arrangements, Bangladesh’s health data ecosystem remained highly fragmented in the past (see Box 3).
Box 3: Bangladesh’s Silent Revolution in the Routine Health Information SystemPrevailing situation: Data generated by private and public-sector providers were not linked and, within the public sector, data from urban and rural areas, and from family planning programmes, were handled separately. Multiple overlapping reporting systems result in heavy paperwork burdens and poor data quality. Partners: GIZ and DHIS2 Results:
Lessons Learned: The comprehensive and systemic approach to HIS strengthening in Bangladesh has shown that it is possible to bring about a more orderly, harmonised information environment even in the absence of an overarching HIS strategy or policy framework. By adopting a pragmatic and incremental approach to modernising the HIS infrastructure, the MIS unit at the Directorate General of Health Services has catalysed a process of change that is leading to a more effective HIS. |
Source: Karen Birdsall, A Quiet Revolution: Strengthening the Routine Health Information System in Bangladesh: A publication in the German Health Practice Collection (Deutsche Gesellschaft für Internationale Zusammenarbeit, November 2014).
Sri Lanka
According to WHO, Sri Lanka is one of the three countries within BIMSTEC—along with Thailand and Bhutan—that have made good progress in placing the strengthening of primary healthcare-oriented health systems at the centre of UHC.[33] Its efforts at integrating occupational health as a component of the public health services is something India can learn from.
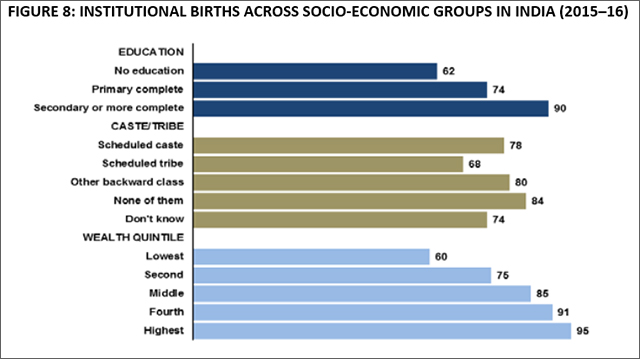
In addition to Thailand, Sri Lanka was the first to achieve the MDG goal on maternal mortality among the BIMSTEC countries. It is acknowledged that the fall in maternal mortality in these countries has largely been due to the increase in the number safe deliveries, i.e., births attended by skilled birth attendants. Sri Lanka could be the best performer mainly because it made efforts at dealing with inequities in access to skilled birth attendants within the country.[34] In India, severe inequalities in access to safe deliveries (see Figure 8) hindered the overall mortality improvements. Figure 8 has data on ‘institutional delivery’, which is slightly different from ‘safe delivery’. However, the spread of the numbers will be quite similar since there are not a great number of non-institutional safe deliveries in India. Latest figures for safe delivery—disaggregated across socio-economic variables—are awaited as unit-level data from NFHS 4 has not yet been made public.
Sri Lanka has a well-established system of maternal death audits, and maternal deaths are notifiable by law. In India, states such as Kerala and Tamil Nadu have implemented maternal death audits, and results have led to systemic changes.[35] The success of Sri Lanka’s efforts at integrated approach to vector management, which led to the elimination of Malaria, should urge India to try community-based measures, integrating chemical and environmental management, thus reducing reliance on pesticides.
Box 4: Sri Lanka’s Multisectoral Approach: A Success StorySri Lanka has achieved one of the lowest child mortality rates among lower-middle income countries. The country has made continuous progress over the past four decades due to a combination of cross-sector public policies that have ensured universal access to education for women, clean water and improved sanitation to the majority, and health system developments that have guaranteed universal coverage of essential preventive and curative health interventions to all women and children. The coverage of deliveries by skilled personnel is 98 percent; coverage with measles, diphtheria, pertussis and tetanus vaccine 97 percent; and the country has the highest breastfeeding rates in the region. It has also been declared Malaria-free. |
Source: http://apps.who.int/iris/handle/10665/204724.
Myanmar
In Myanmar, health system comprises a pluralistic mix of public and private systems, both in terms of financing and provision. The government used to be the main source of financing, with provision of services nearly free until 1993, when user charges were introduced. Later, household out-of-pocket (OOP) payments became the primary source of finance.[36] However, in the last decade, there has been a dramatic turnaround, and between 2007 and 2014, public health expenditure as a percentage of GDP increased by more than six times. Public health expenditure as a percentage of total health expenditure, too, increased by more than five times in the same period, mostly during the last three years.[37] The fresh infusion of funds is expected to help transform the health system marred by inadequate managerial capacity and a lack of proactiveness among health personnel.[38] This is expected to address the problem of stark health inequalities within regions as well, a problem similar to India’s. Myanmar’s health sector improvements are also aided substantially by foreign aid, which has become almost 22 percent of overall health expenditure (2014), from a very low 1.37 percent in 2005.[39]
Conclusion
BIMSTEC proves to be a useful learning opportunity as India’s large and diverse health challenges do not have a singular, centralised solution. In terms of the health challenges being faced by India, the country has vast regions that resemble Thailand, while other areas are similar to Nepal; some states are similar to Sri Lanka, and still others are similar to Myanmar, where internal conflicts create an impact on the government’s ability to deliver quality services. Thailand and Sri Lanka have managed to effectively deal with massive outbreaks of dengue, keeping the mortality low, and many Indian states can learn from their experience. Building capacity for emergency preparedness and response is another area where BIMSTEC members can closely cooperate.
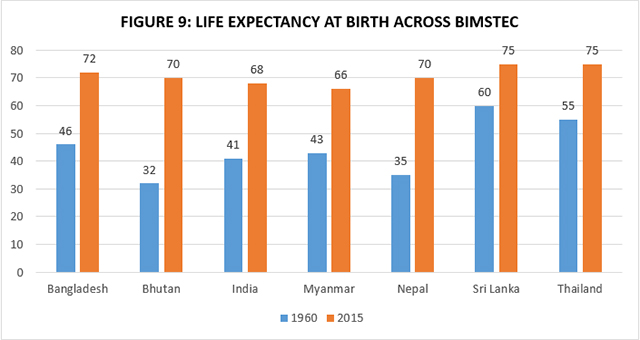
On an average, most of the other BIMSTEC countries have done better than India in terms of verifiable health gains. Gains in life expectancy have been massive in the BIMSTEC region (see Figure 8). The only two countries—Bhutan and Nepal—that had a lower life expectancy than India in 1960 have already overtaken India. Currently, India has the lowest life expectancy in the BIMSTEC region, barring Myanmar, a country torn by internal conflict, but which had a better life expectancy than India in 1960. Given India’s steady economic performance and its size, this situation is quite unfortunate. It calls for introspection, collaboration and cross-learning with BIMSTEC neighbours that have done much better than India in the health sector. An earlier analysis by WHO had shown that life expectancy improvements in the South East Asian region were largely a result of public sector pro-health and pro-poor policies.[40]
There are multiple areas within healthcare where BIMSTEC countries can learn from each other: telemedicine in Bhutan; monitoring of vital events through information technology in Bangladesh; the trial-and-error experimentation with the mother and child tracking system in India; the transformed district health information system in Bangladesh (often called a “silent revolution”); or the hugely useful electronic medical records system in Sri Lanka.[41]
There have been various in-depth, comparative analyses of BRICS country health systems that offer valuable policy lessons.[42] No such study of the BIMSTEC countries exists. The usual self-flagellation in the Indian media while comparing BRICS health data may not be based on objective reality, as India is the poorest country within BRICS by a huge margin.[43] It would do well for India to conduct and support comparative health system studies within BIMSTEC, as the members with stronger economies can offer lessons for the future, and the poorer members can offer lessons for the present.
Cynics may say that India’s slow progress in social indicators when compared to some of its BIMSTEC neighbours is the cost of having a thriving democracy. While that remains arguable, what is certain is that India can learn immensely from these culturally and socially similar neighbouring countries’ successes, as well as their mistakes in health policy.
[1] Vulimiri Ramalingaswami, Urban Jonsson and Jon Rohde, “The Asian enigma,” The Progress of Nations, UNICEF, 1996.
[2] “BIMSTEC: The Road Ahead,” RIS, 2016.
[3] http://www.mea.gov.in/bilateral-documents.htm?dtl/28862/Joint+Statement+of+the+15th+BIMSTEC+Ministerial+Meeting+August+11+2017.
[4] http://pib.nic.in/newsite/PrintRelease.aspx?relid=122888.
[5] http://www.thehindu.com/news/cities/puducherry/bimstec-telemedicine-network-launched/article19273183.ece.
[6] http://nmcn.in/jbtn.php.
[7] http://www.thehindu.com/news/cities/puducherry/bimstec-telemedicine-network-launched/article19273183.ece.
[8] Jyoti Prakash, 2016, http://www.ris.org.in/node/1321.
[9] https://data.worldbank.org/indicator/NY.GDP.PCAP.CD?end=2016&start=1980.
[10] Jean Drèze and Amartya Sen, An uncertain glory: India and its contradictions (Princeton University Press, 2013).
[11] Ibid.
[12] Ibid.
[13] http://www.who.int/workforcealliance/media/qa/05/en/.
[14] https://www.orfonline.org/research/political-policy-lessons-thailand-uhc-experience/.
[15] https://www.ncbi.nlm.nih.gov/pubmed/21227499.
[16] Dina Balabanova, Martin McKee and Anne Mills, eds., ‘Good health at low cost’ 25 years on: What makes a successful health system? (London: London School of Hygiene and Tropical Medicine, 2011).
[17] Suriwan Thaiprayoon and Suwit Wibulpolprasert, “Political and Policy Lessons from Thailand’s UHC Experience,” Issue Brief 174 (New Delhi: Observer Research Foundation, 2017);
[18] http://data.worldbank.org/indicator/SH.XPD.OOPC.TO.ZS?end=2015&locations=TH-LK-BD-BT-IN-MM-NP&name_desc=false&start=1960&view=chart.
[19] http://apps.who.int/iris/bitstream/10665/255701/1/9789290225843-eng.pdf.
[20] http://www.searo.who.int/entity/health_situation_trends/health_int_sdg.pdf.
[21] Ibid.
[22] http://apps.who.int/iris/handle/10665/204724.
[23] Suriwan Thaiprayoon and Suwit Wibulpolprasert, op. cit.
[24] http://unicef.in/PressReleases/219/Global-Data-Sheet and http://blogs.worldbank.org/health/south-asia-s-quest-reduced-maternal-mortality-what-data-show.
[25] http://www.who.int/pmnch/knowledge/publications/nepal_country_report.pdf.
[26] http://apps.who.int/iris/handle/10665/204724.
[27] http://apps.who.int/iris/bitstream/10665/204724/1/B5003.pdf.
[28] Krishna P. Paudel, Lee M. Hampton, Santosh Gurung, Rajendra Bohara, Indra K. Rai, Sameer Anaokar, Rachel D. Swift and Stephen Cochi, “Adapting Nepal’s polio eradication programme,” Bulletin of the World Health Organization 95, no. 3 (2017): 227.
[29] http://apps.who.int/iris/handle/10665/204724.
[30] Corrina Moucheraud, Helen Owen, Neha S. Singh, Courtney Kuonin Ng, Jennifer Requejo, Joy E. Lawn and Peter Berman, “Countdown to 2015 country case studies: what have we learned about processes and progress towards MDGs 4 and 5?” BMC Public Health 16, no. 2 (2016): 794.
[31] http://apps.who.int/iris/handle/10665/204724.
[32] http://health.bmz.de/ghpc/case-studies/A_Quiet_Revolution/index.html.
[33] http://apps.who.int/iris/bitstream/10665/204724/1/B5003.pdf.
[34] Katy Scammell, Douglas J. Noble, Kumanan Rasanathan, Thomas O’Connell, Aishath Shahula Ahmed, Genevieve Begkoyian, Tania Goldner et al., “A landscape analysis of universal health coverage for mothers and children in South Asia,” BMJ Global Health 1, no. 1 (2016): e000017.
[35] http://apps.who.int/iris/bitstream/10665/204724/1/B5003.pdf.
[36] http://www.wpro.who.int/asia_pacific_observatory/hits/series/myanmar_health_systems_review.pdf.
[37] http://data.worldbank.org/indicator/SH.XPD.PUBL?end=2015& locations=MM&name_desc=false&start=1960&view=chart.
[38] http://www.wpro.who.int/asia_pacific_observatory/hits/series/myanmar_health_systems_review.pdf.
[39]http://data.worldbank.org/indicator/SH.XPD.EXTR.ZS?end=2015&locations=MM&name_desc=false&start=1960&view=chart.
[40] http://apps.searo.who.int/PDS_DOCS/B3226.pdf.
[41] A Decade of Public Health Achievements in WHO’s South-East Asia Region, WHO, http://apps.searo.who.int/PDS_DOCS/B5003.pdf.
[42] http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(14)60075-1/abstract; http://www.who.int/bulletin/volumes/92/6/13-127951/en/ , http://csnbricsam.org/wp-content/uploads/2015/04/FINAL-Health-Spending-and-Inequality-E-Gomez.pdf; http://onlinelibrary.wiley.com/doi/10.1111/1758-5899.12340/abstract; https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4407477/; http://onlinelibrary.wiley.com/doi/10.1002/hec.3406/full.
[43] http://data.worldbank.org/indicator/NY.GDP.PCAP.PP.KD?end=2015&locations=IN-ZA-RU-CN-BR&name_desc=false&start=1960&view=chart.
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.

Oommen C. Kurian is Senior Fellow and Head of Health Initiative at ORF. He studies Indias health sector reforms within the broad context of the ...
Read More +