-
CENTRES
Progammes & Centres
Location

On January 30, 2020, the first case of the mysterious Novel Coronavirus, originating in Wuhan, China, was detected in Kerala, India. The spread of this infectious disease in India caused panic due to the country’s image of being an ‘unhealthy nation’. Experts feared that by August, millions could die.
The ‘cardiac capital’ and the ‘diabetes capital’ of the world, India was considered a fertile breeding ground for the pandemic. The Indian population was seemingly more susceptible to the impact of the Novel Coronavirus, due to a high number of people suffering from lung diseases, heart diseases, diabetes, and malnutrition-related conditions, amongst many other ailments. Adding to this fear was that the only known preventive measure for the spread of the coronavirus—the practice of physical distancing—was an almost impossible feat for India, considering that on an average every sixth Indian lives in slums with high population densities, poor environmental sanitation and overcrowded medical infrastructure. In totality, when the pandemic began, predictions for India’s future were usually termed ‘a recipe for disaster’.
Over the past half year, the virus has spread to 98 percent of India’s districts, with more than half the districts reporting 500 or more cases and counting. As the older hotspots in India—mainly consisting of the metro cities such as Delhi, Mumbai, and Ahmedabad—showed cases plateauing, newer hotpots have emerged. Cases in India have now crossed 2.7 million, with more than 50,000 deaths. In July 2020 alone, the country witnessed an almost tripling of cases and doubling of deaths.
While the surge in cases and deaths, when viewed in isolation, can be unsettling, a closer scrutiny of the data has highlighted two key facts. Firstly, while Covid-19 deaths in India have been surging compared to Western countries, India’s case fatality ratio remains low. Secondly, even as Covid-19 deaths have increased, causing a high level of panic and anxiety amongst the citizens, the average daily number of Covid-19 deaths remain considerably lower than deaths from a range of other diseases including Tuberculosis.
As India continues to grapple with the pandemic, research has unveiled a somewhat reassuring fact—that while the Coronavirus is highly transmissible, the fatality rate of the disease is seemingly lower compared to other diseases. The initial results of the serosurvey conducted by the Indian Council of Medical Research (ICMR) to measure the extent of the spread of the virus, revealed that the Infection Fatality Rate (IFR) in India remains low at 0.08 percent. When compared to the infection fatality rates of previous infections, such as the 34% for Middle Eastern respiratory syndrome (MERS), 9.7% for severe acute respiratory syndrome (SARS), 2.5% for Spanish Flu 1918, or 1.3% for H1N1 2009/10 (swine flu), this seems meagre.
As the Coronavirus continued to spread, it was noticed that developed nations such as the USA, UK, Italy and France, have a high Lag-case fatality ratio (L-CFR, a measure of case fatality ratio that removes the effect of lag between reporting and death on data) compared to the global ratio of 5 percent, in addition to bearing a higher number of Coronavirus deaths per million population. The recent flattening curve of cases and deaths in these countries suggests significant progress in stabilising the spread of the pandemic, though a second wave of the pandemic is expected. On the contrary, countries with high population density, which makes it difficult to maintain physical distancing norms, such as India, China, and Brazil, have observed low mortality rates, based on reported deaths data.
While India reported its first Coronavirus case within a 7-day window of Italy, the UK, Germany or Spain finding theirs, India’s case and fatality trajectory has been much slower that its counterparts. Though India is now the third most infected country in the world, with a 12 percent contribution to global cases, the contribution to the global deaths, at 7 percent, remains relatively low—a figure which was unexpected for the second most populated country with a rather weak health infrastructure. On the other hand, countries like the UK, Italy and France, with a much lower contribution to global cases, witnessed a relatively high contribution to the global deaths (5 percent, 5 percent and 4 percent respectively), along with a high case fatality ratio and deaths per million population (Figure 1).
Figure 1: Lag-Case fatality ratio of Top 10 countries (based on Covid-19 deaths)
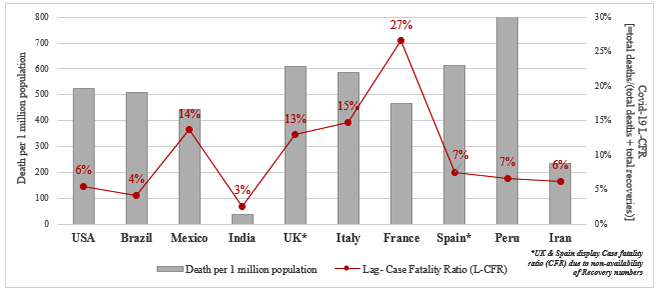 Source: Worldometers, Data as of 1500 hrs, August 18, 2020.
Source: Worldometers, Data as of 1500 hrs, August 18, 2020.
This trend, when observed with the high numbers of people who are part of the ‘at-risk population’ in India, has left many confused. On the one hand, India’s positive trajectory could be attributed to the timely lockdown and India’s young population. On the other hand, the positive trajectory could also be a result of under-reporting of deaths (especially in the case of deaths with co-morbidities), limited testing, and the reluctance to visit hospitals due to the attached social stigma or high costs to healthcare.
While these trends display a more optimistic scenario than many predicted, India must remain vigilant. The high burden of communicable diseases and malnutrition, and the relatively high child and maternal mortality rate – all of which will be amplified and exacerbated by Covid-19—coupled with an inadequate health system in India, pose a serious threat to the future of the country, which may lead to long-lasting shocks to the overall health of its people.
India’s heavy burden of disease has been no secret. In 2017, almost 27,000 people died in India every day, amounting to a total of ~9.7 million fatalities that year. Almost 26 percent of these were caused by communicable, perinatal, maternal, and nutritional diseases. A disease such as Tuberculosis, which has been plaguing India for decades, alone contributes to 43 deaths per hour, amounting to a total of 375,000 deaths in 2017.
A closer look at the top diseases leading to low life expectancy in India reveals that Diarrhea, one of the most prevalent communicable diseases, causes 1,422 deaths every day, whereas ischemic heart diseases and chronic respiratory diseases, such as Asthma, together cause a shocking 6540 deaths on a daily basis.
Figure 2: Estimated Daily Deaths caused by Top diseases in India (2017) and Coronavirus
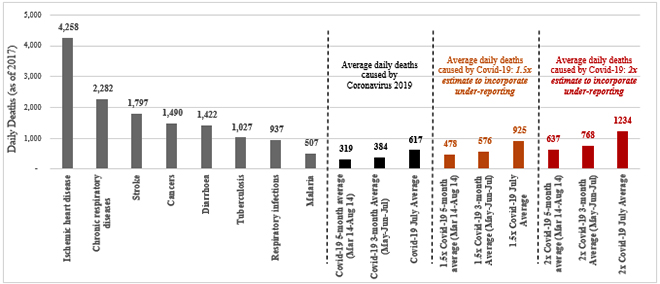 Source: The Lancet National Burden Estimates of healthy life lost in India, 2017.
Source: The Lancet National Burden Estimates of healthy life lost in India, 2017.
The mean daily deaths caused by the novel Coronavirus in India in the past 5 months is 319 (as of August 14), with a daily average of 617 deaths in July alone. The country witnessed a concerning rise in the number of deaths in July, as a result of the virus spreading to new areas. However, a holistic evaluation reveals that these figures still seem lower compared to most other causes of deaths in India. Diseases such as Diarrhea, Tuberculosis and Malaria, for which treatment processes are available, cause more deaths on a daily basis. The level of panic observed during this pandemic has not been seen while countering diseases such as Ischemic heart disease, Diarrhea or Tuberculosis, which have caused many more fatalities and have been burdening the health system of India for decades now.
In this analysis, we have applied a 1.5x and 2x multiplier to the recorded Covid-19 deaths to compensate for the effects of possible undercounting of deaths. Recent evidence suggests that multiple countries undercount the total number of fatalities. Indian experts agree that a 1.5x-2x multiplier should on the average account for the reporting bias, testing inadequacies or co-morbidities. When comparing other causes of death to the estimated 5-month daily average and 3-month daily average deaths caused by Covid-19, the contrast is unmistakable. It is important to note that if the trend observed in the month of July continues and the number of fatalities climb up further, we may have a major cause of worry, until a vaccine is readily available.
A disturbing possibility, which is buried under the cacophony around “Covid-19 issues” and seldom discussed during this pandemic, is the possibility of a sharp rise in non-Covid-19 deaths in the country, due to the current disruptions in healthcare and essential services. While necessary to slow the spread, the stringent lockdown has impacted the mental and physical wellbeing of Indians and has escalated economic losses. Furthermore, as the Coronavirus spread its wings across the country, multiple non-Covid related medical procedures were suspended, with most hospitals being overwhelmed by the Covid-19 patient load. Such a scenario has left the system vulnerable to the impact of other diseases.
As India moved from a stringent lockdown regime towards reopening the country, it has been witnessing a considerable geographical spread and growth in Covid-19 cases and fatalities. Since the initiation of Unlock-1 on June 1, the cumulative average daily cases in India have risen from 2408, as of the 1st June, to 16,386 as of 14th Aug; whereas the cumulative average daily deaths have risen from 68 to 319, in the same time period. As restrictions begin to ease, India, like other countries, must tread carefully due to the unpredictable nature of the virus. While containing the novel Coronavirus is necessary, it is imperative that we ensure that the pandemic does not undo the gains India has made against fighting other diseases in the last decade, which would lead to an unhealthier post-Covid world.
(This article acknowledges the inputs shared by an anonymous reviewer)
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.

Kriti Kapur was a Junior Fellow with ORFs Health Initiative in the Sustainable Development programme. Her research focuses on issues pertaining to sustainable development with ...
Read More +