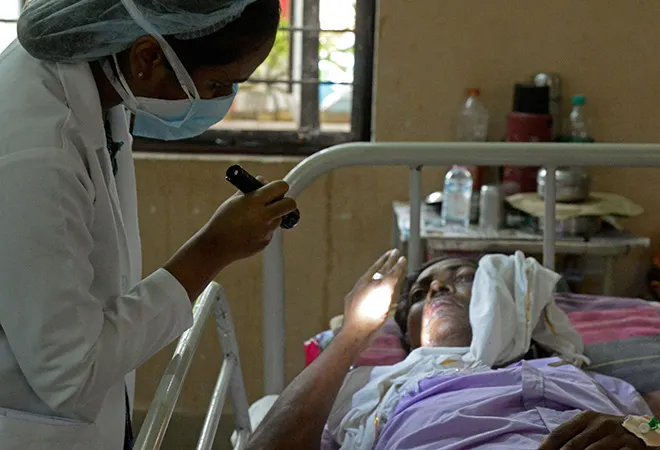
The entire nation has been grappling with the second wave of COVID-19. While this wave should have waned by now, it seems to have entered a self-perpetuating cycle owing to the negligent attitude of the janta, sorry state of an already crippled healthcare system and flawed planning on behalf of the policymakers. As the spread of the virus surged to new highs during this second wave, it also mutated rapidly. Thanks to the second lockdown, increased testing capacity and massive vaccination drive, the number of cases are coming down in most parts of the country, but just when doctors think they have gotten a grasp on this infection, the virus displays baffling manifestations, leaving them dumbfounded.
The “Face” of Death—Mucormycosis
Thousands of people “cured” of COVID-19 have started coming back with complaints of black discharge from the nose or black patches on the face. While it may appear intriguing to most, it is scary to those who have seen and treated it before. This is the usual presentation of Mucormycosis, an invasive systemic fungal infection caused by a group of fungi called Mucorales. The Union Health Ministry has made Mucormycosis a notifiable disease while seven states have already declared it as an epidemic. Mucor wards have been opened alongside COVID wards in the capital of the country. While we lack an accurate data set on its incidence owing to the difficult diagnosis and subsequent under reporting, India has more than 4,000 cases as of May 22, and these numbers are expected to increase exponentially.
Why should we take this seriously? Firstly, all individuals affected with COVID-19 are at risk of this complication, irrespective of severity of the infection. Secondly, its diagnosis is often delayed leading to incorrect or neglected care. Most importantly, the mortality rate of Mucormycosis is 50-100 percent depending on the severity, which implies that more than half of the people affected by it won’t survive.
The Case of Black and White Fungi
Black Fungus refers to Mucormycosis (caused by Mucorales group) while White Fungus refers to another deadly fungi called Aspergillus and Candida. These fungi can affect multiple organs in our body, but each group has its own predilection for certain organs. Patients of COVID-19 are susceptible to infection from both these groups; the mortality rate of black fungus being much higher than its white counterpart. Mucorales are ubiquitous in nature and are found in almost every household. They thrive on any organic matter like fruits and vegetables, roadside wet waste as well as the dead and decaying plants or animals. These fungi release their spores, which are airborne and travel to distant places. As a result, each one of us has been exposed to them multiple times in our life. The tropical climate of our country is a perfect environment for them to grow. Many hospitals across the country have revealed heavy mold spore count in their wards in surveillance studies.
All individuals affected with COVID-19 are at risk of this complication , irrespective of severity of the infection
Why don’t we all get this infection despite exposure? The answer is simple—a strong immune system. Almost every case of Mucormycosis has a risk factor that has weakened the immune system rendering it incompetent to fight against this fungus. The list of risk factors is exhausting but many of them are important in this pandemic. COVID-19 is a viral infection, which is itself known to cause immune system dysfunction. Many patients affected with COVID have other comorbidities like diabetes, kidney disease, liver disease, and cancer, amongst others. The mainstay of COVID treatment today consists of steroids and other high end immunosuppressants like tocilizumab. Lastly, we cannot ignore the high prevalence of malnutrition in our population which weakens the immune defenses.
Once acquired, Mucormycosis mostly affects the face, nose or eye (rhino-orbital mucormycosis) and causes necrosis (death) of the affected tissue. It manifests as blackish discharge from the nose, loosening of teeth, swelling on one half of the face, blackish discoloration of facial skin, eye pain, headache, amongst other symptoms. It can even progress to affect the brain (cerebral mucormycosis) leading to devastating consequences like seizures or paralysis. The treatment of this fungal infection is more complex than its diagnosis. It consists of surgery of the face, eye or brain to remove the adherent mold followed by antifungal medicines for more than a month. It has a tendency to recur and warrants a second surgery in some cases. White fungus (Aspergillus), on the other hand, usually affects the lungs (invasive pulmonary aspergillosis) and leads to worsening respiratory distress, hemoptysis (blood in sputum) and respiratory failure, if left unattended.
Having said that, the most astounding fact is that India has recorded the highest number of Mucormycosis cases in this pandemic, much more than all other countries combined. We still do not have a concrete explanation for this discrepancy.
Black Fungus or a Black Swan?
The emergence of black fungus is actually a black swan event which became obvious in hindsight. Although it is described as ‘rare’ in western literature, India in the pre-COVID era contributed to 40 percent of the global burden with an estimated 140 cases of Mucormycosis per million population. This tells us that our country was already a hotbed for fungal infections. India is also the well-known diabetes capital of the world with more than 40 million cases. It has been shown that 47 percent of Indians are unaware of their diabetic status and only a quarter of them are appropriately treated. If we look at the population across the board, many Indians are malnourished (which includes both under and over nourishment). Thus, our country was already primed for the boom of fungal infections. The COVID-19 pandemic pulled the trigger and caused immune dysfunction on a mega scale. The events up to this point were largely out of our control.
Although it is described as ‘rare’ in western literature, India in the pre-COVID era contributed to 40 percent of the global burden with an estimated 140 cases of Mucormycosis per million population
Where did we go wrong?
- All cases of COVID-19 requiring oxygen support need to be given steroids for at least 10 days as shown by the RECOVERY trial of the UK. Steroids are powerful drugs that can halt the immune dysfunction being caused by the virus. Sadly, many doctors in every corner of the country have misused these guidelines and prescribed steroids to those who were not seriously ill. On top of it, patients started self medicating with steroids owing to their over-the-counter availability and low price in our country. Consequently, a large proportion of cases took steroids even when they didn’t need it and the unsupervised prescriptions led to irrational doses and duration of steroid intake. This could have been prevented by sensitisation of doctors regarding the importance of guidelines as well as emergency restriction on dispensing of steroids by pharmacists.
- An important risk factor conveniently forgotten by most patients and caregivers is the glucose (sugar) levels in the blood. Steroids have the potential to increase the blood glucose level in any person. Increased glucose in the blood creates a favourable milieu for fungal growth. Millions of diabetics with COVID-19 were treated with steroids while less attention was paid to the strict control of their blood glucose levels. People who were not diabetic were not followed up subsequently for a delayed rise in blood glucose. As a result, a large chunk of patients ended up with high blood sugars and steroids in their blood.
- Surprisingly, oxygen therapy is one of the potential culprits too, but in a specific and different way. While oxygen has to be given to patients who need it, care has to be taken regarding its source and humidification. Owing to the acute shortage of medical grade oxygen across the country, the Empowered Group II under the Government of India directed all major oxygen manufacturers to convert industrial grade oxygen cylinders for medical use. They have also been directed by state governments to convert nitrogen/argon cylinders into oxygen cylinders. Industrial oxygen production and storage is not done under strict asepsis as required for medical grade oxygen, thus, carries a significant risk of contamination with microbes including bacteria and fungi. Although there are SOPs for these procedures, whether the manufacturers, cylinder handlers, transport personnel and distributors followed the precautions rigorously or not is a highly debatable topic. Inside the hospitals, the water used to humidify the oxygen is another potential source of contamination. In an environment where molds are already present, any laxity in the manufacturing or humidification, under work-stress or timeline-pressure, can have serious consequences.
- Delayed diagnosis in this pandemic is because of varied reasons, one of which is self-medication at home with alternative medicines while ignoring genuine medical advice. It has been observed that many people resort to alternative therapies instead of consulting medical doctors leading to inadvertent progression of the disease.
Since the recognition of this new epidemic, we have been witnessing another round of passing the parcel of blame between governmental and non-governmental agencies, including hospitals and doctors; the initial round being played at the beginning of the COVID-19 pandemic. As expected, everyone has again resorted to finding the “elixir” for Mucormycosis instead of focusing on the simpler preventive measures. Amphotericin B, the only medicine known to effectively combat black fungus, has gone out of stock in many places and is being already sold under the table. It is soon going to be the next Remdesivir for opportunistic profiteers if not regulated.
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.




 PREV
PREV


