Goal three of the ambitious Sustainable Development Goals (SDGs) requires all countries to achieve Universal Health Coverage(UHC) by 2030. This entails access to quality essential health care services, access to safe, effective and affordable medicines and vaccines, as well as financial risk protection for all at all ages. UHC could, therefore, be regarded as an umbrella goal for health in the new development agenda. The importance of this particular target cannot be overemphasized – it not only transcends all other health-related targets but also draws linkages with the rest of the development goals. The achievement of UHC is critical to the success of the overarching vision of the SDGs, which is to ‘leave no one behind’. Given the population size and health burden of India, one can also posit that the global accomplishment of the SDGs is contingent on India’s success.
While healthcare has witnessed considerable progress over the past decade, the pace of improvement has been slow and plagued with a multiplicity of challenges. In fact, a Lancet study published last week ranks India 127th in terms of meeting the United Nations health-related SDGs – lowest among its BRICS peers (Figure 1). It is obvious therefore, that India’s fast economic growth has not yet translated into the health sector in a significant way. To ensure sustained growth levels, the country requires a strong and healthy workforce – possible only when citizens are protected against health-related financial risks and canaccess quality health services. If India is really serious about goal three, as it should be given that health is a fundamental building block for growth and development of the country, it needs to address certain issues that currently act as a road-block towards the accomplishment of UHC.
Figure 1: Performance on the health-related SDG index among BRICS countries
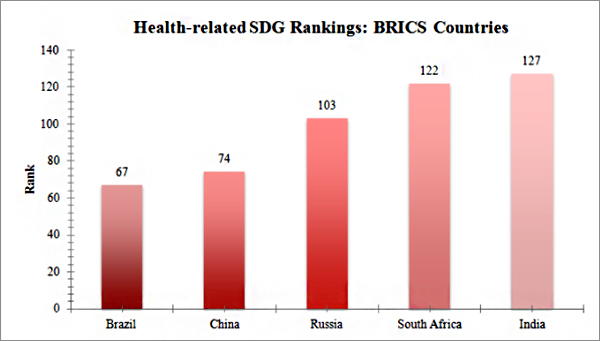 Source: Global Burden of Disease Study 2016
Source: Global Burden of Disease Study 2016
It is first and foremost imperative to look at UHC through a gender lens. Contrary to the layman understanding of gender, this does not imply a discussion on women’s health alone but an approach to UHC which is inclusive in nature and attends to the needs of men and women.
What is needed is a shift in narrative – the onus of a woman and child’s health is not on women alone but on the entire society. Addressing such issues requires going beyond health and delving into challenges that arise from societal attitudes, gender discrimination when it comes to nutrition, education and sanitation. Given the patriarchal society we live in, gender equity in health would need approaches that are much more women-centric and supportive of their multiple roles. These social determinants and root causes should be recognized while framing policies to extend UHC in the country.
Next, achieving UHC requires long-term high-level political commitment. This has unfortunately been absent in the Indian context. At a macro level, the government spends a measly proportion (1.18 percent) of its Gross Domestic Product (GDP) on health – among the lowest globally. The long-awaited National Health Policy (NHP) 2017 proposed to increase public health spending to 2.5 percent of GDP by 2025. This is disappointing to say the least given that eight years from now India intends to continue spending well below the current world average of 5.99 percent. Together with low public sector investments in health, the system also suffers from poor coordination caused by the presence of a vast number of vertical health programmes (many of which deal with similar issues) and several institutions within the health department that must work together if they are to deliver anything worthwhile. This often leads to bureaucratic apathy and inertia, which tends to slow down delivery of healthcare services and hampers the smooth functioning of the healthcare system.
Finally, given that the private sector is the largest provider of healthcare services in the country, it would be impossible to achieve the 2030 goals without its active involvement.
The government, however, should always take lead as no country has ever built a successful health system devoid of a central authority. The challenge is in defining the role that the government wants the private sector to play in the provision of healthcare and how it can ensure that funds are spent in a better way. One way to do this would be through price control, as already done with stents. This is an effective tool to extend quality health services at affordable prices. Other such mechanisms need to be explored and implemented to maintain a balanced participation from the private sector.
Way Forward
While it may be tempting to follow the path which other countries have embarked upon to achieve UHC, it is important to remember that India has its own unique challenges and therefore requires context specific solutions. Within the country too, certain states are performing exceptionally and so rather than looking outside for lessons, Indian should look inwards and take lessons from the successes and failures of its states.
Access, affordability and quality are central to the UHC theme. Given the crucial role of private sector in the healthcare delivery system, India needs to begin seriously finding an ideal mix of public private investments.
It would also help to clearly define and distinguish the purview of public and private sectors within the health system. The government should leverage private sector resources to fill in the healthcare delivery gaps. Resource allocation is a critical decision that also needs to be taken. Speaking at a high-level consultation organised by the Observer Research Foundation and the Bill and Melinda Gates Foundation, Mr. C.K. Mishra, Health Secretary, stated that majority of resources should be directed towards “primary healthcare, to preventive and promotive health. It does not make sense to go on increasing hospital beds and simultaneously go on increasing the number of patients in the country. Therefore, all policies must converge on getting investment into primary healthcare”. In fact, the NHP released this year calls for two-third resources to flow into the primary health sector.
Whether investments should flow from public or private sectors and how much? Where should resources be allocated? How can underlying socio-economic issues causing gender inequities be addressed? How can government accountability and transparency be maintained to ensure political commitment for UHC? – Often asking the right questions is more important than finding answers. In order to redesign the Indian healthcare system so as to make it conducive to UHC, India needs to first recognise its failures. Perhaps it is time for a dose of realism – identifying gaps and flaws will only help find viable solutions and lead to informed policy-making.
This commentary originally appeared in Economic Times.
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.




 Source: Global Burden of Disease Study 2016
Source: Global Burden of Disease Study 2016 PREV
PREV


