
Most of the great pandemics in recent recorded history have lasted several years.
• The Antonine Plague of 165 AD afflicted and devastated the Roman Empire. The Emperor of Rome Marcus Aurelius also succumbed to it. It continued until 180 AD.
• The “black death” pandemic of pneumonic plague too lasted for four years, from 1347 to 1350. It spent considerable time in each area it infested, ravaging the local population completely before moving on to the next.
• Between the years 1831 to 1837, an influenza pandemic swept across Europe in three waves: one each in 1831, 1833 and 1837.
• The Russian Flu of 1889 lasted for almost two years, killing 360,000 people.
• The influenza pandemic of 1899 lasted for five years. Over one lakh British citizens perished in this pandemic.
• The 1918 Spanish Flu influenza pandemic, arguably the most devastating in history, killed an estimated 50 million people in three waves between March 1918 and November 1919. Each wave had as high mortality as the previous one. However, the first outbreaks of this disease had been recorded in 1917 by two separate groups of researchers.
And as you read this article, COVID-19 has entered its third calendar year: the first cases were reported towards the end of 2019, spread across the globe rapidly in 2020 and is raging on in the first half of 2021, having taken over 2.8 million lives worldwide. Going by the history of pandemics, one can say with some degree of confidence that the behaviour of the COVID-19 pandemic is not particularly unusual with regard to its resurgence as “waves.”
Phases of pandemics
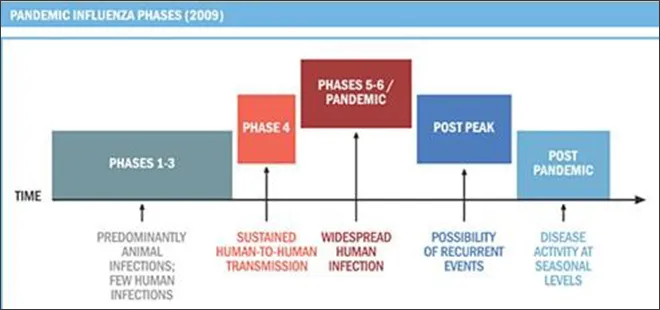
The above chart by the World Health Organisation shows the natural course of pandemics. We are in phases 5-6 of the COVID-19 pandemic, as the number of cases are still rising globally. Most experts agree that COVID-19 too would eventually become a post-pandemic seasonal illness.
Factors responsible for “pandemic waves”
Several factors have been identified for ebb and wave patterns in the transmission of pandemics. Daihai et al. proposed a simple model for the three waves of the 1918 influenza pandemic, that involved:
• Schools opening and closing.
• Temperature changes during the outbreak.
• Changes in human behaviour in response to the outbreak.
Kissler et al. have identified the following factors for the post-pandemic transmissibility of SARS-CoV-2:
• Degree of seasonal variation in transmission.
• Duration of immunity.
• Degree of cross-immunity between SARS-CoV-2 and other coronaviruses.
• Intensity and timing of control measures.
Viral mutation is an additional factor that can lead to fresh outbreaks even in people who have been infected earlier. The SARS-COV2 virus has shown significant mutations and some of the mutant strains have been found to have higher infectivity. India has reported that up to 20% of its fresh cases are from a double mutant strain. The UK and South Africa variants do not seem to have played a major role in India.
The rise and fall in the number of cases is dependent on the complex interaction between these factors. Certain other peculiarities have been identified. For example, studies on the 1918 pandemic suggested that the pandemic hit the poor in the first wave and the rich in the next. This certainly seems to corroborate with the behaviour of the COVID-19 pandemic in the city of Mumbai, where the first wave devastated the slums while the second one is raging chiefly in the high-rises.
Learning from history
The traditional methods of control of pandemics have remained virtually unchanged for several centuries:
• Isolation and treatment of infected persons.
• Containment of disease spread through quarantine measures.
• Personal protective barriers.
• Proper communication and spread of information to the population at large.
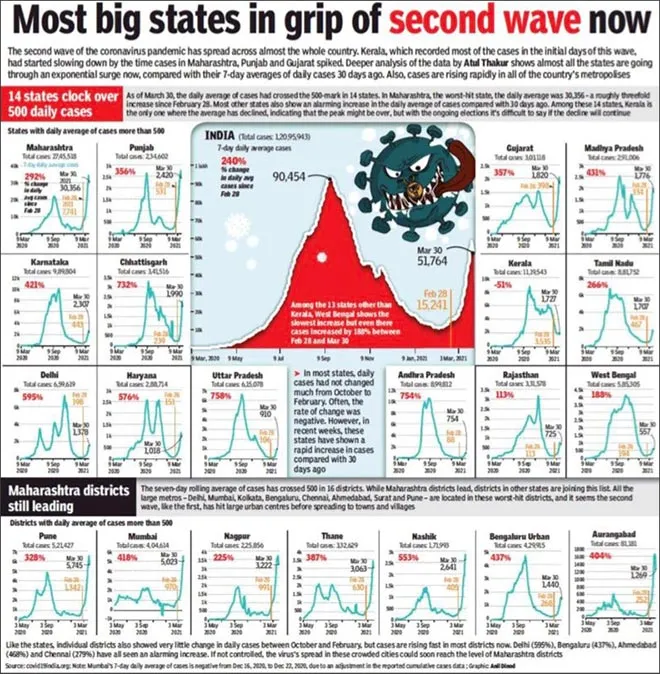
Failure in proper implementation of one or more of these factors leads to loss of control over the situation. And there have been several failures on this front, as a result of which India is now in the grip of a huge second wave. Though the bulk of cases are from Maharashtra, several states are showing a sharp increase in the number of fresh cases.
The provisions of the Epidemic Act are still in force throughout the country, and there are restrictions on mass gatherings in most states. However, the restrictions have been repeatedly, blatantly and publicly violated. A fact-finding team from Central government visited Maharashtra and found that the causes for the present second wave were most likely “Covid-inappropriate behaviour due to lack of fear of disease, pandemic fatigue; miss outs and super spreaders; and enhanced aggregations due to recent gram panchayat elections, marriage season and opening of schools, crowded public transport, etc.”
In short, every principle of pandemic management has been thrown to the winds.
The political class is guilty of holding huge political rallies in the middle of a raging pandemic. The current outbreak of COVID-19 that has gripped Maharashtra started immediately after intensive local campaigning for Panchayat elections across the state throughout January 2021. West Bengal is already showing a huge spike in the number of fresh cases following huge rallies by various political parties. Assam has not shown any significant increase, probably owing to the fact that there were only around 515 active cases in the entire state during the time the rallies were held. In any case, it does not help that lakhs of people are seen gathering together, most of them without masks, in mega rallies that are highly televised. The hard lessons of history, such as the 1918 devastation of Philadelphia due to influenza following a large parade, have obviously not been learnt.
Every principle of pandemic management has been thrown to the winds.
In several states such as Punjab, Bihar and Maharashtra, the so-called “wedding season” has resulted in a series of super-spreader events. Hundreds of people crammed in an airconditioned hall in which people partied without masking or distancing during an ongoing pandemic, was always going to be an invitation for disaster. In sharp contrast, the Uttar Pradesh government proactively took several preventive measures at the start of the “wedding season” and escaped relatively unscathed. The state has also been relatively alert and strict on quarantine and isolation measures for patients and contact tracing.
In Maharashtra, extended public transport timings and creation of additional transport facilities were needed to decompress the usually heavily congested public transport. However, while capacities were augmented by introduction of additional buses and trains, for some inexplicable reason, the state government decided to restrict timings to just a few hours, leading to massive overcrowding. The same blunder was repeated several times, first by keeping local trains closed and overburdening the bus network, and later by restricting timings of public transport for the general population to just a few hours a day. The reopening of schools also resulted in cluster outbreaks in several states.
Proper communication and spread of information to the population, that was excellent throughout the early stages of the pandemic, has also suffered. The drop in the number of cases led to a number of articles that claimed India would not see a second big wave of COVID, and that we were already close to herd immunity. The messaging from the Central government too seemed to suggest that we had beaten back COVID-19. This seems to have had a ripple effect on the population. Biased media coverage was considered a key factor in the failure to contain the 1918 pandemic.
The political class is guilty of holding huge political rallies in the middle of a raging pandemic.
Some experts, too, jumped in prematurely and claimed that India would not see a second wave as it had attained “herd immunity.” Senior government officials admitted that some complacency crept in, leading to lax attitudes towards implementation of control measures. To top this, while the bed occupancy situation in Maharashtra continued to deteriorate rapidly, the state government failed miserably in communicating the seriousness of the situation to its population. In stark contrast to the factual situation where patients were struggling for hours to get a single bed and most large hospitals had waiting lists of patients, the Municipal Commissioner of Mumbai continued making pompous claims that more than enough beds were available for treatment.
Ending the pandemic
Mass vaccination is the only safe and reliable method to end the pandemic without significant mortality. We have several precedents to show that this can be done and that it works. The Asian Flu pandemic of 1957 was stopped in its tracks by vaccination. Outbreaks of Ebola have been contained by mass vaccinating the local population.
With high-risk population being prioritised, the mortality due to COVID would be expected to fall sharply.
As the majority of healthcare workers in India have already been completely vaccinated, mortality rates due to COVID in this high-risk group have plummeted to near zero. The focus of most state governments, therefore, is to mass vaccinate the entire population on a war footing. With high-risk population being prioritised, the mortality due to COVID would be expected to fall sharply. It would be desirable to authorise several other vaccines and procure as many doses as possible, for this purpose.
As the vaccine efficacy is around 80%, some people can still develop COVID post-vaccination but mortality is very rare. In Israel, where over 60% of the population has now received at least one dose of the vaccine, life has more or less returned to the pre-pandemic normal. It is heartening that less than 3% of ICU admissions for severe COVID in Israel were patients who had been fully vaccinated as against 75% who had not received even a single dose of the vaccine. There is considerable data to show that vaccination protects against mutant strains, although in variable degrees. The elimination of mortality due to COVID would effectively reduce this virus to the status of a seasonal common cold. That is a good goal to have.
The views expressed above belong to the author(s). ORF research and analyses now available on Telegram! Click here to access our curated content — blogs, longforms and interviews.






 PREV
PREV


